1. Introduction and overview
1.1. Introduction
1.1.1. The popularity of traditional medicine
The use of traditional medicine (TM) containing ingredients obtained from animals and plants has maintained its popularity in all regions of the developing world and is gaining in popularity in the industrialised countries. Countries in Africa, Asia and Latin America use TM to help meet some of their primary health care needs while in industrialised countries, traditional medicine use is seen as “Complementary“ or “Alternative” (CAM) to orthodox or allopathic medicine. Thus, in Africa, up to 80% of the population uses traditional medicine for primary health care and in China traditional herbal preparations account for 30%–50% of the total medicinal consumption. In Europe, North America and other industrialised regions, over 50% of the population have used complementary or alternative medicine at least once. The popularity of TM has created a global market for herbal medicines that currently stands at over US $ 60 billion annually and is growing
steadily (WHO, 2004).
1.1.2. The threat to endangered species from their use in traditional medicine
The growing market in TM poses a major threat to the survival of many endangered species, notably tigers, bears and rhinoceroses. Most TM “consumer” countries, including China, Japan, the UK and the USA, are Parties to the Convention on International Trade in Endangered Species (CITES), which bans international trade in these species between CITES member states. However, demand for medicines containing them continues and with it illegal trade in their parts and derivatives for the TM market. Tigers, rhinoceroses, and three species of bear, are listed under CITES Appendix 1 (2004); species that are the most endangered among CITES-listed animals and plants and are threatened with extinction. Despite this protection, the number of tigers, bears and rhinoceroses in the wild continues to fall. Tiger numbers have dropped from more than 100,000 to between 4,800 and 7,300 individuals over the last century, three tiger species have become extinct, and, as tigers become increasingly difficult to find, other big cat species have begun to be hunted as an alternative. Whilst several parts of the tiger are used in TM, tiger bone is the most commonly used. It is believed to have an anti-inflammatory effect, particularly in cases of arthritis.
Bear populations are also declining around the world to the extent that the immediate survival of bears in key regions is threatened. It is recognised that bears are poached and illegally traded for use in TM, but the extent of illegal poaching is difficult to assess. Various bear parts are used in Asian TM, including the meat, gall bladder, brain, blood, bone and paw. Bear bile, extracted from the gall bladder, is most commonly used in TM, being prescribed for febrile diseases with high temperature and convulsions, inflammation of the liver, laryngitis, conjunctivitis and to reduce swelling and pain (for trauma, sprains, fractures and haemorrhoids). Rhinoceros populations have also suffered severely in recent years. Three of the five species of rhinoceros are now critically endangered and threatened with extinction, with more that half of the world’s remaining rhinoceroses lost during the 1970s (WWF, 2002). The use of rhinoceros horn in TM has largely been blamed for the decline in the population in Asia. Rhinoceros horn is prescribed in Asian TM as a detoxifying, anti-inflammatory and anti-convulsant agent and is used in the treatment of advanced stages of fever.
1.1.3. The need for research into the use of substitutes for specimens of endangered species
Parties to CITES have expressed concern over the continued and uncontrolled use of several endangered species in traditional medicine in view of the potential threat to the long-term survival of these species and the need to ensure the continued use and development of traditional medicines on a sustainable basis (CITES, 1997; Conf. 10.19). It has been recognised that problems of overexploitation must be addressed within the context of an improved understanding about the significance of traditional medicines in the world’s health care
systems. A resolution was therefore agreed at the 10th meeting of the Conference of Parties 1997 (CITES, 1997) calling for more research into the use of substitutes for specimens of endangered species in TM. The UK, represented by the Global Wildlife Division of the Department for Environment, Food and Rural Affairs (DEFRA), the UK CITES Management Authority, was instrumental in CITES in gaining agreement to this Resolution. IFAW first began to address the issue of endangered species used in traditional medicine products in 1983 and have also emphasised the importance of research into herbal alternatives.
1.1.4. Middlesex University and traditional medicine
Against this background, the increasing popularity of TM in the industrialised countries, including the UK, led to the introduction of degree level education in several TM disciplines. Middlesex University was at the forefront of these developments, validating a degree in Herbal Medicine in 1994 and in Traditional Chinese Medicine (TCM) in 1996. Both programmes aim to provide an education and training to produce graduates who will be competent, reliable and caring practitioners. The TCM programme was developed and is delivered in collaboration with Beijing University of Chinese Medicine. The need to address issues surrounding the use of endangered species in TCM practice and to bring endangered species education into the curriculum is recognised by the academic group at Middlesex, as is the need for appropriate research in this area.
1.2. The current research project
In 2001 DEFRA and IFAW jointly commissioned Middlesex University to undertake research to investigate “Plant Substances as Alternatives for Animal Products Used in Traditional Chinese Medicine”. The research was carried out at Middlesex and at the Jodrell Laboratories, Royal Botanic Gardens, Kew. The Royal Botanic Gardens at Kew are the UK appointed CITES Scientific Authority for Plants and carry out CITES projects and research into the trade in certain CITES-listed plants. In addition, Dr Bing Chan acted as external advisor on matters of TCM philosophy and practice. The project was designed to be carried out in two parts. Project 1 was to investigate anti-inflammatory and anti-pyretic herbs as alternatives for bear bile and rhino horn. Project 2 was to investigate anti-inflammatory and anti-rheumatic herbs as alternatives for
tiger bone. As the project progressed, further collaborations were established in order to achieve the aims of the project. These collaborations are listed in the acknowledgements. All collaborators have been vital to the success of the project and their input greatly valued.
1.2.1. Aims of the project
The overall objective of the project is to provide original scientific data to support the promotion of alternatives to the use of animal products in TM in order to help prevent the further depletion of threatened and endangered wildlife. The original aims for phase 1 and 2 of this research proposal were as follows:
i) To identify the active chemical components of products derived from bear (bile), tiger (bone) and rhino (horn).
ii) Once identified, to find plant substitutes.
The following report summarises the work that has been carried out over the past three years. From the report it can be seen that the initial aims of the project have been met. Having conducted an extensive literature review and consultations with Chinese medicine practitioners, the decision was taken to place the emphasis on the choice of herbs to investigate as possible alternatives to animal products based on TCM theory and philosophy rather than on similarities in chemical structure or in activity in Western pharmacological terms. The latter was taken into account and investigated once the choice of herbs had been made. This decision was taken as the team consider that the effective promotion of the use of alternatives to practitioners and patients of TCM will depend on their acknowledgment that the herbs possess the same or similar properties to the animal products as described by TCM philosophy. Also taken into consideration was the common usage in TCM of prescriptions consisting of a combination of herbs with a ‘principal’ ingredient. Several prescriptions, which include animal products as an ingredient, were therefore also investigated.
All three animal products under investigation (bear bile, rhino horn and tiger bone) are used in TM medicines for a variety of reasons, but all share a common use as an anti-inflammatory. Both bear bile (Xiong Dan) and rhino horn (Xi Jiao) are also classified in TCM as anti-pyretic remedies and tiger bone (Hu Gu) as an anti-rheumatic/anti-arthritic remedy. Herbs chosen for investigation based on TM theory were therefore investigated in vitro for their efficacy as anti-inflammatory agents. Since fever is often initiated by infection (commonly bacteria) anti-bacterial tests were also conducted as part of the bear bile and rhino horn projects. There has been concern expressed over possible herb-herb and drug-herb interactions and over the contamination of herbal medicines with metals and pesticide residues. This was investigated using cytochrome P450 3A4 assays, and quantitatively evaluating the chemical contaminants (metals and pesticide residues) in some selected herbs. In addition, the importance of authentication of herb samples is recognised and the plant species of the herbs in this study was investigated using chemical analysis. An additional suggestion, though not included in the initial proposal for funding, was the possibility of extending the research to include animal trials, followed by human trials using volunteers to assess the effectiveness of herbal alternatives (Phase 4). It has not been felt that there is justification at this point to extend the project in this way and that this would, in any
case, conflict with the mission and vision of both the University and the funding bodies.
1.3. Structure of the report
The report is divided into 7 sections. Following this overview, Sections 2, 3, and 4 present the rationale for the selection of herbs to investigate as potential alternatives to bear bile, rhinoceros horn and tiger bone respectively, identifying both herbs and combinations of herbs (prescriptions) chosen and briefly describing their properties as identified in the literature. Section 5 describes the methods used to prepare, authenticate and assess the biological activity of the chosen herbs. The assays allowed investigation of anti-bacterial activity, anti-inflammatory activity (NF−κΒ inhibition) and cytochrome P450 3A4 activity. Section 6 presents the main findings of the investigation into biological activity. The results of assays to measure contaminant levels (pesticide residues and metals) are shown in Appendices 2, 3A and 3B. A summary of the main findings and suggested future work is outlined in Section 7.
2. Rationale for selection of herbs as potential alternatives to bear bile
2.1. Introduction
In order to identify which plants might be suitable to replace bear bile use in traditional medicine (TM), in particular, traditional Chinese medicine (TCM), it is important to understand the beliefs and evidence supporting its continued use. In this part of the report, sources of bear bile, its uses in TM and the identification of active constituents used in ‘Western’ medicine are discussed. Based on the findings of this research, the criteria for choosing herbs to investigate as potential alternatives were established, based on both the traditional uses and knowledge about medicinal properties of the different species of plants. Whilst single herbs have been selected for study, it is recognised that a mixture of different plant species is commonly prescribed in TCM, with the prescription relying on purported synergism of a combination of herbs, sometimes with animal parts and minerals. Therefore, prescriptions or combinations of herbs were also investigated as potential
alternatives to the use of bear bile in TCM. A summary of some of the known constituents and available research on the herbs and prescriptions chosen for study as potential alternatives to the use of bear bile in TCM is given at the end of this section.
2.2. Sources of bear bile
In TCM, bear bile was originally obtained from two members of the Ursidae family, namely, Selenarctos thibetanus (Asiatic black bear) and Ursus arctos (brown bear) (Bensky and Gamble, 1993; Chang and But, 1987). There is evidence to suggest that other species of bears such as Ursus americanus (American black bear) and Helarctos malayanus (sun bear) have also been exploited (Lin et al., 1997). Selenarctos thibetanus (Ursus thibetanus), Helarctos malayanus and Melursus ursinus (sloth bear) are among bear species listed under CITES Appendix 1 (2004), banning international trade in their parts in CITES member states. However, due to demand for bear products in TCM, regulated bear farming is in operation in China and the Republic of Korea, where bile is artificially drained from bear gall bladders (Li, 2004). As a substitute to bear bile, bile derived from pig, water buffalo, goat, cattle and chicken have also been used in TCM and several of these have been sold as ‘bear bile’ (Lin et al., 1997).
2.3. Bear bile and its constituents in TCM and Western medicine
Bear bile is composed of deconjugated tauroursodeoxycholic acid (TUDC), taurochenodeoxycholic acid (TCDC) and taurocholic acid (TC), of which the primary bile acids are known as ursodeoxycholic acid (UDCA), chenodeoxycholic acid (CDCA) and cholic acid, respectively (Espinoza et al., 1993). In the UK, pharmaceutical products containing UDCA (e.g. Destolit, Urdox, Ursofalk, Ursogal), which may be obtained from other animal sources (e.g. ox), are indicated for the dissolution of gallstones (British Pharmacopoeia, 2000). UDCA has also been used in the treatment of some chronic inflammatory disorders such as liver fibrosis and chronic active hepatitis (Kowdley, 2000; Rolo et al., 2000; Van
Den Bogaert, 2003).
2.4. Bear bile in TCM
Bear bile (Xiong Dan; Fel Ursi) is described in TCM as having a ‘bitter’ taste and being ‘cold’ in nature. There are several ailments associated with the use of bear bile (Bensky and Gamble, 1993; Chang and But, 1987). These include gallstones, cholestatic hepatic diseases, febrile diseases with high fever and convulsions, pharyngolaryngitis, conjunctivitis, traumatic injuries, swelling, pain, sprains and fractures, haemorrhoids and cardiovascular diseases. The Association of Chinese Medicine and Philosophy and Earthcare Society (Hong Kong) in their report on ‘Herbal alternatives to bear bile in Chinese medicine’ included syphilis and several cancers as being treated by bear bile (IFAW report, 1994). Bile obtained from other species of animals has also been investigated; one study showed bear bile and pig bile to demonstrate comparable anti-inflammatory, analgesic and anti-convulsant properties and therefore, pig bile has been advocated as a suitable animal alternative to bear bile (Li et al., 1995).
2.5. Selection of herbs and herbal prescriptions for investigation
2.5.1. Criteria used for selection of single herbs
There is some scientific evidence to support the traditional use of bear bile in the treatment of inflammatory conditions (Li et al., 1995), and its chief active constituent, UDCA, in the treatment of cholesterol gallstones and chronic liver inflammation (Van Den Bogaert, 2003), some cardiovascular diseases (Lee, 1999) and cancer (Im and Martinez, 2004). At the beginning of this study an extensive literature survey was conducted to select herbs to be investigated as possible alternatives to bear bile. One hundred and three plant species used as ‘heat-clearing’ herbs in TCM were identified. In order to select suitable herbs, criteria were then used which included herbs with constituents similar in structure and function to UDCA, a tetracyclic compound. For example, pentacyclic triterpenoids such as ursolic and oleanolic acid are attributed with anti-inflammatory, hepatoprotective and anti-neoplastic activities (Saraswat et al., 2000; Syrovets et al., 2000). However, these compounds are found in several plant species. In consultation with TCM practitioners, the criteria were further refined (Table 2.1.) in order to select herbs with both TCM and pharmacological properties similar to bear bile.
| Table 2.1. Properties / functions of bear bile and UDCA used as criteria for herb selection | |
| Criteria | Properties and functions of bear bile and UDCA |
| A | ‘Cold’ nature |
| B | ‘Bitter’ taste |
| C | ‘Heat clearing’ |
| D | ‘Fire-purging’ |
| E | Anti-inflammatory properties |
| F | Hepatoprotective properties |
| G | Anti-neoplastic properties |
| H | Cardiovascular protective properties |
Criteria A – D: TCM properties of bear bile (Bensky and Gamble, 1993; Chang and But, 1987).
Criteria E – H: Pharmacological / clinical effects of bear bile and UDCA reported in the literature (Li et al., 1995; Lee, 1999; Van Den Bogaert, 2003; Im and Martinez, 2004).
| Table 2.2. TCM plants selected after consultation with TCM practitioners and from evaluation of TCM literature and pharmacological and clinical data | |||||||||
| Plant species with some similar properties to bear bile | A | B | C | D | E | F | G | H | TCM references |
| 1. Gardenia jasminoides Ellis (syn.: G. augusta Merr.) (Rubiaceae) fruit = Zhi Zi | * | * | * | * | * | * | * | 1, 2, 4 | |
| 2. Anemarrhena asphodeloides Bge. (Anthericaceae) rhizome
= Zhi Mu |
* | * | * | * | * | 1, 2, 4 | |||
| 3. Scutellaria baicalensis Georgi (Lamiaceae) root = Huang Qin | * | * | * | * | * | * | * | 1, 2, 4 | |
| 4. Coptis chinensis Franch. (Ranunculaceae) rhizome = Huang Lian | * | * | * | * | * | * | * | 1, 2, 4 | |
| 5. Phellodendron amurense Rupr (Rutaceae) bark = Huang Bai | * | * | * | * | * | * | 4 | ||
| 6. Andrographis paniculata Nees (Acanthaceae) aerial parts = Chuan Xin Lian | * | * | * | * | * | * | 1, 2, 4 | ||
| 7. Rheum palmatum L. (Polygonaceae) root and rhizome = Da Huang | * | * | * | * | * | 1, 3 | |||
Criteria A – D (refer to Table 2.1.): based on TCM literature (Chang and But, 19871; Bensky and Gamble, 19932;
Chang and But, 20013; Chinese Pharmacopoeia, 20054). Criteria E – H (refer to Table 2.1.): based on pharmacological and clinical data (Section 2.4).
Out of the eight criteria listed (Table 2.1.) priority was given to plant species that complied with the properties of bear bile as described in TCM [Table 2.1; criteria A – D]. Therefore, all the herbs selected for study are traditionally used in the practice of Chinese medicine. Additional criteria for choice were based on evidence from published scientific studies [Table 2.1; E – H]. When assessing the suitability of the selected herbs as alternatives to bear bile, the known relevant biological activities and their constituents were also considered.
The potential for using these species as alternatives to bear bile was then discussed with TCM practitioners. These discussions resulted in a reduction in the number of plant species from 103 species to 7 species (Table 2.2.).
2.1.1. Criteria used for selection of herbal prescriptions for study
In addition to the 7 selected herbs chosen for study, the use of prescriptions in TCM was also considered. In TCM, a mixture of different plant species is commonly prescribed, relying on the synergy between herbs, sometimes with animal parts and/or minerals. A literature survey was therefore conducted on TCM prescriptions containing bear bile with the aim of selecting prescriptions for investigation, to determine whether they demonstrate biological activity without bear bile. A major criterion for choosing TCM prescriptions for this study was that they contained not more than one animal product (i.e. bear bile). It was also important to choose prescriptions that did not contain endangered plant species (those restricted by CITES). A survey identified a TCM prescription (prescription X), which complied with the criteria. Prescription X is used in the treatment of laryngitis and contains bear bile and six herbs (Zhu, 1989). The herbal composition of prescription X is described in Table 2.3. In addition, two Chinese-Japanese (Kampo) patent medicines, Orengedokuto and Diao-Orengedokuto are also proposed as possible replacements for prescriptions containing bear bile. These two prescriptions were selected on the basis of being composed of herbs proposed from this investigation and also possessing some similar biological and TCM functions as bear bile.
| Table 2.3. Herbal composition of prescription X |
| Herbs listed as being in prescription |
| Zhi Zi, fruit of Gardenia jasminoides (Rubiaceae) |
| Huang Lian, rhizome of Coptis chinensis (Ranunculaceae) |
| Ban Lan Gen, root of Isatis indigotica (Brassicaceae) |
| Jin Yin Hua, flower bud of Lonicera japonica (Caprifoliaceae) |
| Lian Qiao, fruit of Forsythia suspensa (Oleaceae) |
| Hu Po, fossil resin of Pinus succinifer (Pinaceae) |
2.2. Single herbs chosen as potential alternatives to bear bile in TCM: summary of reputed and pharmacological effects
2.2.1. Huang Qin (Radix Scutellariae)
Huang Qin (skullcap) is prepared from the root of Scutellaria baicalensis Georgi (Lamiaceae). It functions to ‘remove damp’, ‘quench fire’ and counteract toxins. It is used as an anti- inflammatory agent and in the treatment of fever, hepatitis and acute conjunctivitis (Bensky and Gamble, 1993; Chang and But, 1987). The anti-pyretic, analgesic (Huang
et al., 1990), anti-hypercholesterolemic (Yotsumoto et al., 1997), cardiovascular protective (Wang et al., 2004) and anti-neoplastic (Fukutake et al., 1998; Wozniak et al., 2004) effects of S. baicalensis have been reported. In addition, the anti-inflammatory effect of
- baicalensis has been demonstrated in vitro and in vivo (van Loon, 1997; Cuellar et al., 2001). Flavonoid constituents (baicalein, baicalin, wogonin and oroxylin A) of S. baicalensis have been researched for the mechanism of action of their anti-inflammatory effects (Chen et al., 2000; Chen et al., 2001; Kang et al., 2003a; Huang et al., 2004).
2.2.2. Huang Lian (Rhizoma Coptidis)
Huang Lian (goldthread rhizome) is prepared from the dried rhizome of Coptis chinensis Franch, C. deltoidea C.Y.Cheng.&Hsiao, or C. teeta Wallich (Ranunculaceae). It is used traditionally in the treatment of some inflammatory diseases, fever, conjunctivitis and some tumours (Hsu et al., 1986; Chang and But, 1987). Some studies have associated Rhizoma Coptidis with potential anti-inflammatory, anti-oxidant, anti-hypercholesterolemic, and
anti-neoplastic effects. C. chinensis has shown anti-inflammatory activity in vivo (Cuellar et al., 2001), which may be mediated through the inhibition of interleukin-8 (IL-8) induction (Lee et al., 1995). Berberine, a constituent of C. chinensis, is reported to inhibit cyclooxygenase-2 (COX-2) activity (Fukuda et al., 1999). C. chinensis is reported to be anti-oxidant in vitro and in vivo (Liu and Ng, 2000; Schinella et al., 2002) and has shown cholesterol lowering effects (Yotsumoto et al., 1997; Yokozawa et al., 2003). Rhizoma Coptidis has also shown potential anti-neoplastic effects in vitro (Fukutake et al., 1998;
Iizuka et al., 2000). Anti-bacterial activity of Rhizoma Coptidis is cited in Chang and But (1987) and Tang and Eisenbrand (1992). Adverse effects associated with Rhizoma Coptidis include vomiting, dyspnoea and convulsions (Huang, 1999).
2.2.3. Huang Bai (Cortex Phellodendri)
Huang Bai (Amur corktree) is prepared from the dried stem bark of Phellodendron amurense Rupr. (Rutaceae). It functions as a ‘heat-clearing’, anti-inflammatory and anti-bacterial agent in TCM (Chang and But, 1987; Tang and Eisenbrand, 1992). Some studies indicate that P. amurense has anti-inflammatory (Cuellar et al., 2001), hepatoprotective (Yotsumoto et al., 1997), anti-oxidant (Kong et al., 2001) and anti-bacterial (Chang and But, 1987) activities. In one study, the hepatoprotective effects of Cortex Phellodendri were reported to be less effective than Rhizoma Coptidis and Radix Scutellariae (Yotsumoto et al., 1997).
2.2.4. Zhi Zi (Fructus Gardeniae)
Zhi Zi (cape jasmine fruit) is prepared from the fruit of Gardenia jasminoides Ellis (syn.:
- augusta Merr.) (Rubiaceae). It is reputed to ‘reduce heat’, ‘remove heat from the blood’, counteract toxicity and ease the mind (Pharmacopoeia of PRC, 2000). It is a ‘fire-purging’ febrifuge and is indicated in febrile diseases with restlessness. It is also used traditionally
in the treatment of conjunctivitis, some tumours and externally for sprains and bruises (Chang and But, 1987; Bensky and Gamble, 1993). The anti-inflammatory, anti-neoplastic (Fukutake et al., 2000) and hepatoprotective (Chiu et al., 1989) activities of Fructus Gardeniae have been reported. Genipin and geniposide, constituents of the herb, have been reported to be analgesic (Harada et al., 1974) and geniposide is reported to be anti- inflammatory in vivo (Yao et al., 1991). Genipin, as well as crocetin have been reported to possess anti-neoplastic properties (Chang et al., 1996; Kuo et al., 2004). Fructus Gardeniae and its constituents, genipin and crocin, are reported to be choleretic (Harada et al., 1974; Tang and Eisenbrand, 1992). Crocin, a carotenoid constituent of Gardenia jasminoides possess anti-oxidant properties (Pham et al., 2000). However, reversible acute hepatic damage has been observed with crocin (Tang and Eisenbrand, 1992) and diarrhoea was observed as a side effect of geniposide in mice (Bensky and Gamble, 1993). Gardenic acid and gardenodic acid A (constituents of Gardenia jasminoides) can cause abortion in early pregnancy (Pei-Gen and Nai-Gong, 1991).
2.2.5. Chuan Xin Lian (Herba Andrographis)
Chuan Xin Lian (green chiretta) is prepared from the dried aerial parts of Andrographis paniculata Nees (Acanthaceae). It is used in TCM to ‘remove heat’, ‘counteract toxicity’ and reduce swelling (Pharmacopoeia of PRC, 2000). It is used traditionally in the treatment of inflammatory diseases, fever, hepatitis and pharyngolaryngitis (Chang and But, 1987; Bensky and Gamble, 1993; Hocking 1997). There is some scientific evidence to support the traditional use of A. paniculata as an anti-pyretic, anti-inflammatory, hepatoprotective and cardiovascular protective agent. Clinical trials indicate that A. paniculata has some efficacy in treating fever, sore throat and cold symptoms, but was not as effective as paracetamol (Thamlikitkul et al., 1991; Caceres et al., 1999). Diterpene lactones (andrographolide, neoandrographolide, 14-deoxy-11, 12-didehydroandrographolide
and 14-deoxyandrographolide) from A. paniculata have been reported to exert anti- inflammatory effects through the inhibition of nitric oxide (Zhang and Tan, 1999; Chiou et al., 2000; Batkhuu et al., 2002), and are also reputedly anti-pyretic (Chang and But, 1987). The anti-inflammatory action of andrographolide has been extensively researched (Habtemariam, 1999; Amroyan et al., 1999; Chiou et al., 2000; Shen et al., 2002) and it is also reported to possess anti-neoplastic properties (Rajagopal et al., 2003). The hepatoprotective activities of A. paniculata have been reported (Ram 2001; Trivedi et al., 2001), and several hepatoprotective compounds have been isolated from A. paniculata
(Jain et al., 2000). Extracts of A. paniculata and 14-deoxy-11,12-didehydroandrographolide have demonstrated cardiovascular activity in vivo (Guo et al., 1996; Zhang et al., 1998).
Overdose of the herb may cause dizziness, palpitations, gastric discomfort and loss of appetite (Chang and But, 1987; Huang, 1999). The herb extract has shown contraceptive effects in vivo (Zoha et al., 1989).
2.2.6. Zhi Mu (Rhizoma Anemarrhena)
Zhi Mu is prepared from the dried rhizome of Anemarrhena asphodeloides Bge (Anthericaceae). It is classified as a ‘fire-purging’ anti-pyretic (Pharmacopoeia of PRC, 2000). A. asphodeloides and its constituent, sarsapogenin, are reputed to reduce fever in vivo (Chang and But, 1987; Huang, 1999). A xanthone-C-glucoside isolated from
- asphodeloides, mangiferin, has shown anti-oxidant effects (Sanchez et al., 2000; Ma et al., 2001). Mangiferin and other constituents of A. asphodeloides, cis-hinokiresinol, tigogenin and hecogenin have demonstrated anti-neoplastic properties (Yoshimi et al., 2001; Corbiere et al., 2003; Jeong et al., 2003). A. asphodeloides is reputed to have an inhibitory effect on several bacteria (Chang and But, 1987).
2.2.7. Da Huang (Radix et Rhizoma Rhei)
Da Huang (rhubarb) is prepared from the dried root and rhizome of Rheum palmatum L.,
- tanguticum Maxim. and R. officinale Baill. (Polygonaceae). It is used traditionally mainly as a laxative and also in the treatment of haemorrhoids, conjunctivitis and as a choleretic
agent (Hsu et al., 1986; Tang and Eisenbrand, 1992; Huang, 1999). Radix et Rhizoma Rhei has been shown to have cholesterol reducing effects through the inhibition of 3-hydroxy- 3-methlyglutary-coenzyme A (HMG-CoA) reductase activity (Kim et al., 2002). The rhizome of R. undulatum and constituent stillbenes (rhapontigenin, piceatannol, resveratrol, chrysophanol 8-O-b-D-(6’-galloyl)-glucopyranoside and aloe-emodin 1-O-b-D- (glucopyranoside) have been shown to exert anti-inflammatory effects through the inhibition of nitric oxide production in vitro (Matsuda et al., 2000; Kageura et al., 2001).
Species of Rheum used in Da Huang listed above have shown anti-oxidant effects in vitro
(Matsuda et al., 2001b)
2.3. Prescriptions chosen for investigation as potential alternatives to bear bile in TCM
2.3.1. Orengedokuto
Orengedokuto (Huanglian-Jie-Du-Tang, TJ-15) is a traditional kampo patent medicine which is approved as an ethical medicine by the Ministry of Health and Welfare of Japan, and is listed in the Pharmacopoeia of Japan for the treatment of cerebrovascular disease, hypertension, gastritis and liver diseases (Ohta et al., 1998; Maclean and Taylor, 2000). Orengedokuto is composed of four herbs (Table 2.4.).
In this current study, the four herbs were individually studied and proposed as herbal alternatives to bear bile. There has been extensive scientific research, by other workers, into the pharmacological properties of Orengedokuto. Similar to bear bile, it has been associated with anti-inflammatory (Dai et al., 2000; Fukutake et al., 2000), hepatoprotective (Ohta et al., 1998; Seikiya et al., 2002) and anti-neoplastic (Fukutake et al., 2000) effects.
| Table 2.4. Composition of herbs in Orengedokuto (Seikiya et al., 2002) | |
| Herbs | Ratio |
| Huang Qin (Radix Scutellariae) | 3.0 |
| Huang Lian (Rhizoma Coptidis) | 2.0 |
| Huang Bai (Cortex Phellodendri) | 1.5 |
| Zhi Zi (Fructus Gardeniae) | 2.0 |
Water extracts of Rhizoma Coptidis, Radix Scutellariae and Fructus Gardeniae (three of the components of orengedokuto) also showed some potential anti-neoplastic activity, but with lower efficacy than the formula (Fukutake et al., 1998; Fukutake et al., 2000). Fructus Gardeniae has also been associated with potential anti-inflammatory activity (which may be mediated via inhibition of COX-2 activity) (Fukutake et al., 2000). Orengedokuto has also been reported to inhibit hepatic cholesterol ester formation by inhibiting the activity of acyl-coenzymeA:cholesterol acyltransferase (ACAT) in vitro (Yotsumoto et al., 1997). In addition, extracts of Radix Scutellariae, Rhizoma Coptidis and Cortex Phellodendri decreased ACAT activity, whereas Fructus Gardeniae had no significant effect (Yotsumoto et al., 1997). However, oral administration of Orengedokuto was not able to significantly reduce fever caused by a bacterial pyrogen in vivo (Itami et al., 1992).
2.3.2. Dia-Orengedokuto
Dia-Orengedokuto contains the same herbs as Orengedokuto with an additional herb, Radix et Rhizoma Rhei and is used in the treatment of atherosclerosis (Kim et al., 2002). Water and ethanol extracts of Dia-Orengedokuto inhibited the activity of HMG-CoA reductase more potently than extracts of Orengedokuto (Kim et al., 2002). Of the herbal constituents of Dia-Orengedokuto, Rhizoma Coptidis was more potent at reducing HMG- CoA reductase activity, followed by Radix et Rhizoma Rhei (Kim et al., 2002). Constituents of bear bile (CDCA and cholic acid) are also inhibitors of HMG-CoA reductase, which leads to reduction in hepatic cholesterol levels (Björkhem et al., 1993).
2.4. Alternatives to bear bile: summary
Based on both traditional uses and knowledge of the medicinal properties of the different species of plants, a selection of 7 single herbs and 2 prescriptions consisting of a combination of herbs, were chosen as alternatives to bear bile in TCM. In addition, a TCM prescription containing bear bile was considered for study (prescription X). From Table 2.2., it is apparent that none of the 7 herbs listed as having similar properties to bear bile fulfil all the functions reputedly associated with bear bile. In addition, some TCM prescriptions containing bear bile also contain some of the suggested herbal replacements. It may be that, in some circumstances combinations of herbs, based on TCM principles, may be more suitable as replacements for bear bile in prescriptions containing the animal product.
The Association of Chinese Medicine and Philosophy and Earthcare Society (Hong Kong) has published a report on ‘The Herbal Alternatives to Bear Bile in Chinese Medicine’ based on TCM philosophy (IFAW report, 1994). They suggest 54 herbs as alternatives to bear bile (Appendix 1). Five of the seven herbs listed in Table 2.2 were also proposed in the IFAW report as alternatives to bear bile, Huang Qin (Radix Scutellariae), Huang Bai (Cortex Phellodendri), Zhi Zi (Fructus Gardeniae), Chuan Xin Lian (Herba Andrographitis) and
Da Huang (Radix et Rhizoma Rhei). The underlying pathology of several of the ailments treated with bear bile is inflammation. In humans, inflammation is often initiated by infection, frequently caused by different species of bacteria (Moltz, 1993). Therefore, in this study, the herbs and prescription selected for investigation as possible alternatives to bear bile were tested in anti-bacterial and anti-inflammatory assays. The methods used and the results obtained in the present study are presented in Sections 5 and 6.
3. Rationale for selection of herbs as potential alternatives to rhino horn
3.1. Introduction
This section addresses the selection of potential herbal alternatives to rhino horn in TCM. As with the choice of herbs to investigate as potential alternatives for the use of bear bile, selection has been based on investigation of both traditional use and the medicinal properties of the different species of plants. In this part of the report, sources of rhino horn, its uses in TCM and its reported pharmacological activities are discussed. In addition, TCM prescriptions traditionally containing rhino horn were investigated to determine their pharmacological potential in the presence and absence of the animal product. A summary of some of the known constituents and available research on the herbs and prescriptions selected for further investigation is given.
3.2. Sources of rhino horn
The black rhino (Deceros bicornis, Rhinocerotidae) population decreased by 95% between 1970 and 1993 (WWF, 2002). Due to a decline in their population, all five species (Deceros bicornis, Cerathotherium sinum, Dicerorhinus sumatrensis, Rhinoceros sondaicus, Rhinoceroos unicornis) of Rhinocerotidae are listed under CITES Appendix 1 (2004), therefore banning international commercial trade in their parts. Water buffalo horn has been used as an animal substitute for rhino horn, but generally at higher doses (Bensky and Barolet, 1990). Other alternatives to rhino horn include horns from cattle and the Saiga antelope (But et al., 1990).
3.3. Rhino horn and its constituents
The primary constituent of rhino horn is keratin; constituents also include other proteins, amino acids, peptides, sterols, amines and calcium (Ingaki and Oida, 1970; Lee and Kim, 1974; Chang and But, 1987). Aqueous extracts of horns from rhino, Saiga antelope (Saiga tatarica), water buffalo (Bubalus bubalis) and cattle (Bos taurus domesticus) are reported to be anti-pyretic (But et al., 1990). But and Tam (1991) investigated the anti-pyretic properties of herbal prescriptions containing either rhino horn or buffalo horn; separate rhino and buffalo horn extracts were found to be anti-pyretic and the combined horn-herb
extracts were also anti-pyretic. In another study, rhino horn did not show anti-pyretic activity in vivo (Laburn and Mitchel, 1997). But et al. (1990) cited other studies conducted in Asia on the anti-pyretic properties of rhino horn with contradictory conclusions, but mainly with negative results. Scientific research into the anti-pyretic properties of rhino horn has shown that it is effective at reducing temperature in febrile animals only at high concentrations.
3.4. Rhino horn in TCM
In TCM, rhino horn is considered as having a strong action of ‘clearing heat’, ‘removing heat from the blood’, as well as arresting convulsions (Xu, 1994). The low efficacy of the rhino horn extracts to reduce temperature in febrile animals could in part be explained by the differences in concepts of the pathology of fever between Western medicine and TCM. The major difference is that in TCM febrile diseases can manifest without an increase in body temperature (Hsu et al., 1986; Xu, 1994). In contrast, febrile diseases are associated with an increase in body temperature in Western medicine (Moltz, 1993).
Rhino horn (Xi Jiao; Cornu Rhinocerotis) is used as a detoxifying, anti-convulsant and anti-inflammatory agent. A major use of rhino horn is in the treatment of advanced stages of fever in the ying and blood conformation, complicated by delirium or coma. It is often used in combination with other TCM remedies and the horn is reputed to be a potent anti-convulsant in these remedies (Chang and But, 1987). Haemorrhagic conditions (e.g. erythema, haematemesis and epistaxis) sometimes manifest symptoms associated with conditions treated by rhino horn. Rhino horn has also been associated with the treatment of cardiovascular diseases (Chang and But, 1987).
3.5. Selection of herbs and prescriptions for investigation
3.5.1. Criteria used for selection of single herbs
After consulting TCM practitioners a set of criteria was developed (Table 3.1.) and used to conduct a survey of TCM literature, to identify herbs to be investigated as possible alternatives to rhino horn (Table 3.2.). This was used in consultation with TCM practitioners to select nine plant species (Table 3.2.) for further investigation.
| Table 3.1. Properties / functions of rhino horn used as criteria for herb selection | |
| Criteria | Properties and functions of rhino horn |
| A | ‘Cold’ nature |
| B | ‘Bitter’ taste |
| C | ‘Salty’ taste |
| D | ‘Blood cooling’ |
| E | ‘Heat clearing’ |
| F | Anti-convulsant |
| G | Anti-inflammatory properties |
| H | Anti-pyretic properties |
| I | Reduce haemorrhage |
| Table 3.2. TCM herbs selected after consultation with TCM practitioners and from evaluation of TCM literature and pharmacological and clinical data | ||||||||||
| Herbs with some similar properties to rhino horn | A | B | C | D | E | F | G | H | I | TCM references |
| 1. Scrophularia ningpoensis Hemsl. (Scrophulariaceae) root
= Xuan Shen |
* | * | * | * | * | * | * | 1, 2 | ||
| 2. Rehmannia glutinosa Steud (Scrophulariaceae) root
= Sheng Di Huang |
* | * | * | * | * | 1, 2 | ||||
| 3. Paeonia suffruticosa Andr. (Paeoniaceae) root = Mu Dan Pi | * | * | * | * | * | * | 1, 2 | |||
| 4. Paeonia veitchii Lynch or P. lactiflora Pall. (Paeoniaceae) root
= Chi Shao |
* | * | * | * | * | * | * | 2 | ||
| 5. Arnebia euchroma I.M.Johnst. (Boraginaceae) root = Zi Cao | * | * | * | * | * | 1 | ||||
| 6. Isatis indigotica (Brassicaceae) root = Ban Lan Gen | * | * | * | * | * | * | 1, 2 | |||
| 7. Lonicera japonica Thunb. (Caprifoliaceae) flower bud
= Jin Yin Hua |
* | * | * | * | * | 1, 2 | ||||
| 8. Forsythia suspensa Vahl (Oleaceae) fruit = Lian Qiao | * | * | * | * | * | 1, 2 | ||||
| 9. Salvia miltiorrhiza Bge (Lamiaceae) root = Dan Shen * | * | * | * | 1, | 2 | |||||
Criteria A – I (refer to Table 3.1.): based on TCM literature (Bensky and Gamble, 19931; Chinese Pharmacopoeia, 20052).
3.5.2. Criteria used for selection of herbal prescriptions
When combined with other TCM remedies to form prescriptions, rhino horn is reputed to play an important role. Therefore, another literature survey was conducted to ascertain TCM prescriptions containing rhino horn, which could be studied in biological assays with and without rhino horn. Five TCM prescriptions were selected for study on the basis of containing rhino horn as the only animal component. The prescriptions selected were Qing Ying Tang, Qingwen Baidu Yin, Xi Jiao Dihuang Tang, Sheng Xi Dan and Qing Gong Tang. Also selected was a TCM prescription composed only of herbs, Zhi Zi Jin Hua, which was used as a TCM ‘control’. All six prescriptions are used to treat epidemic febrile diseases and their compositions are described in Table 3.3.
| Table 3.3. The distribution of 23 herbs and one mineral in six TCM prescriptions. | ||||||
| TCM control | TCM prescriptions traditionally containing rhino horn | |||||
| Zhi Zi Jin Hua | Qingwen Baidu Yin | Xi Jiao Dihuang Tang | Qing Ying Tang | Sheng Xi Dan | Qing Gong Tang | |
| 1. Xuan Shen, root of Scrophularia ningpoensis (Scrophulariaceae) | * | * | * | * | ||
| 2. Sheng Di Huang, root of Rehmannia glutinosa (Scrophulariaceae) | * | * | * | * | ||
| 3. Mu Dan Pi, root of Paeonia suffruticosa Andr. (Paeoniaceae) | * | * | ||||
| 4. Chi Shao, root of Paeonia lactiflora, P. veitchii (Paeoniaceae) | * | * | ||||
| 5. Zi Cao, root of Arnebia euchroma (Boraginaceae) | * | |||||
| 6. Ban Lan Gen, root of Isatis indigotica (Brassicaceae) | * | |||||
| 7. Jin Yin Hua, flower bud of Lonicera japonica (Caprifoliaceae) | * | * | * | |||
| 8. Lian Qiao, fruit of Forsythia suspensa (Oleaceae) | * | * | * | * | ||
| 9. Dan Shen, root of Salvia miltiorrhiza (Lamiaceae) | * | |||||
| 10. Zhi Mu, rhizome of Anemarrhena asphodeloides (Anthericaceae) | * | * | ||||
| 11. Zhi Zi, fruit of Gardenia jasminoides (Rubiaceae) | * | * | ||||
| 12. Huang Qin, root of Scutellaria baicalensis (Lamiaceae) | * | * | * | |||
| 13. Huang Lian, rhizome of Coptis chinensis (Ranunculaceae) | * | * | * | |||
| 14. Huang Bai, cortex of Phellodendron amurense (Rutaceae) | * | |||||
| 15. Da Huang, root and rhizome of Rheum palmatum (Polygonaceae) | * | |||||
| 16. Tian Hua Fen, root of Trichosanthes kirilowii (Cucurbitaceae) | * | * | ||||
| 17. Lian Zi Xin, seed of Nelumbo nucifera (Nelumbonaceae) | * | |||||
| 18. Mai Men Dong, root of Ophiopogon japonicus (Convallariaceae) | * | * | ||||
| 19. Dan Zhu Ye, aerial part of Lophatherum gracile (Poaceae) | * | * | * | |||
| 20. Jie Geng, root of Platycodon grandiflorum (Campanulaceae) | * | |||||
| 21. Gan Cao, root of Glycyrrhiza uralensis or G. glabra (Leguminosae) | * | |||||
| 22. Chang Pu, rhizome of Acorus calamus, A tatarinowii (Acoraceae) | * | |||||
| 23. Dan Dou Chi, seed of Glycine max (Leguminosae) | * | |||||
| 24. Shi Gao, calcium sulphate | * | |||||
| Zhi Zi Jin Hua was used as a TCM control prescription in biological tests. Herbs numbered 1 to 7 are also listed in Table 2.6 as possible alternatives to rhino horn. | ||||||
The six prescriptions were made up of a total of 23 herbs and one mineral (Table 3.3.). It became apparent from Table 3.3., that all nine possible herbal ‘alternatives’ to rhino horn already existed in one or more prescriptions used in this study. This finding confirmed the practice in TCM of combining remedies with similar functions for their additive and synergistic effects. However, it challenged the logic of replacing one plant species with a specific range of functions with another species that has different properties, and that might already exist in a prescription. Therefore, the principles governing the composition of TCM prescriptions were considered in determining the suitability of the selected herbs as alternatives to rhino horn.
3.1. Single herbs as potential alternatives to rhino horn: reputed and pharmacological effects
3.1.1. Ban Lan Gen (Radix Isatidis)
Ban Lan Gen (Dyer’s woad) is prepared from the dried root of Isatis indigotica Fort. (Brassicaceae). Similar to rhino horn, it is a ‘blood cooling’ febrifuge with the TCM properties ‘cold’ and ‘bitter’ (Hsu et al., 1986). Ban Lan Gen is used traditionally as an anti-inflammatory, anti-bacterial and anti-viral remedy, and is often used in the treatment of seasonal febrile diseases (Hsu et al., 1986; Ho and Chang, 2002). Ho and Chang (2002) reported that the methanolic extract of the dried roots of I. indigotica was anti-pyretic, anti-inflammatory and analgesic. Ethanol extracts of the roots of I. indigotica and organic acids isolated from I. indigotica (2-aminobenzoic acid, benzoic acid, salicylic acid, syringic acid and 3-(2’-carboxyphenyl)-4(3H)-quinazoline) showed anti-endotoxin activity (Wu et al., 1997). The alkaloid tryptanthrin, isolated from I. indigotica, inhibited nitric oxide, PGE2 (Ishihara et al., 2000) as well as 5-lipoxygenase (5-LOX) and COX-2 activities (Danz et al., 2002), indicating anti-inflammatory properties. Isaindigotone, also an alkaloid from I. indigotica, inhibited 5-LOX activity, prostaglandin E2 (PGE2) generation and nitric oxide (Molina et al., 2001).
3.1.2. Chi Shao (Radix Paeoniae Rubra)
Chi Shao is prepared from the dried roots of Paeonia lactiflora Pall. (white peony) or P. veitchii Lynch (red peony) (Paeoniaceae). Similar to rhino horn, it is classified as a ‘blood cooling’ febrifuge in TCM (Hsu et al., 1986; Wiseman and Ye, 1998). It has been reputed to possess analgesic and anti-convulsive effects (Hsu et al., 1986; Ding et al., 2000). P. lactiflora and its constituent paeonol, are reported to be anti-oxidant (Goto et al., 1999; Ohsugi et al., 1999). P. lactiflora demonstrated anti-inflammatory action in vitro (Huang et al., 1990) and reduced liver damage in vivo (Qi, 1991). Radix Paeoniae Rubra showed anti-neoplastic properties in vitro (Lee et al., 2002). Paeoniflorin isolated from P. lactiflora has been shown to be an anti-hyperlipidemic agent in vivo (Yang et al., 2004), reduce haemorrhage due to bacterial infection and possess anti-inflammatory properties in vitro (Ding et al., 2000). Another compound, 1,2,3,4,6-penta-O-galloyl-b-D-glucose isolated from the root of Paeonia lactiflora has been shown to possess anti-oxidant, anti-neoplastic and anti-inflammatory effects (Lee et al., 2003). Resveratrol, also isolated from the root of Paeonia lactiflora, has been reported to have anti-oxidant and anti-neoplastic activities, in vitro (Kang et al., 2003b).
3.1.3. Mu Dan Pi (Cortex Moutan)
Mu Dan Pi is prepared from the dried root bark of Paeonia suffruticosa Andr. (Paeoniaceae). Similar to rhino horn, it is used as a ‘blood-cooling’ febrifuge in TCM (Hsu et al., 1986; Wiseman and Ye, 1998). The TCM herbs Mu Dan Pi and Chi Shao have been shown to have some similar pharmacological and phytochemical properties (Lin et al., 1999; Ding et al., 2000). Both herbs contain the compounds paeoniflorin, resveratrol and 1,2,3,4,6-penta-O-galloyl-b-D-glucose (pharmacological properties are listed under Chi Shao). Recently, 1,2,3,4,6-penta-O-galloyl-b-D-glucose has been demonstrated to exert anti-inflammatory activity through the inhibition of IL-8 via NF-kB binding inhibition (Oh et al., 2004) and inhibition of iNOS and COX-2 (Lee et al., 2003). The major lipophilic compound from P. suffruticosa, paeonol and minor constituents, 2,5-dihydroxy-4- methoxyacetophenone and 2,5-dihydroxy-4-methylacetophenone have also demonstrated anti-inflammatory effects (Lin et al., 1999). Methanolic extracts of P. suffruticosa inhibited IL-8 production (Oh et al., 2003); water extracts showed anti-oxidant effects (Liu and Ng, 2000), in vitro. Some compounds from P. suffruticosa namely suffruticosides A, B, C, and D, galloyl-oxypaeoniflorin, and galloyl-paeoniflorin has been reported to exhibit more potent anti-oxidant effects than a-tocopherol (Matsuda et al., 2001a).
3.1.4. Dan Shen (Radix Salvia Miltiorrhizae)
Dan Shen (red sage root) is prepared from the root of Salvia miltiorrhiza Bge (Lamiaceae). Tanshinones from S. miltiorrhiza are reported to be anti-inflammatory in rats with infective arthritis (Duke and Ayensu, 1985) and in mice with croton oil induced inflammation of the ear (Tang and Eisenbrand, 1992), however the mechanism of action was not established in these studies. A diterpene, tanshinone IIA, isolated from the root of S. miltiorrhiza demonstrated anti-inflammatory effects through the inhibition of iNOS expression and production of TNF-a, IL-1b and IL-6 (Jang et al., 2003). Tanshinones from S. miltiorrhiza root have also demonstrated anti-inflammatory activity in mice and were active against
- LOX in porcine leukocytes, but were not as active as the crude extracts (Chang and But, 1986; Paulus and Bauer, 2000).
3.1.5. Jin Yin Hua (Flos Lonicerae)
Jin Yin Hua (honeysuckle) is prepared from the dried flower buds of Lonicera japonica Thunb. (Caprifoliaceae). It is used traditionally as an anti-bacterial, anti-inflammatory and anti-pyretic remedy (Chang and But, 1987; Tang and Eisenbrand, 1992). A water extract of L. japonica demonstrated anti-inflammatory properties by inhibiting NF–kB activity, inducible nitric oxide and TNF-a in vitro (Lee et al., 2001); anti-inflammatory effects of aqueous extracts of L. japonica have also been shown in vivo (Tae et al., 2003). Oral administration of a butanol extract of L. japonica had mild anti-inflammatory activity against acute granulomatic and chronic inflammatory models in vivo (Lee et al., 1998).
Other studies provide some information regarding the compounds that might be responsible for the anti-inflammatory effects of the crude extracts. Lonicerosides A and C, saponins from the aerial parts of L. japonica, caused inhibition of ear oedema in vivo (Kwak et al., 2003). Some compounds (e.g. methyl caffeate, 3,4-di-O-caffeoylquinnic acid, methyl 3,4-di-O-caffeoylquinate) isolated from L. japonica, inhibited platelet aggregation (Chang and Hsu, 1992); methyl caffeate and methyl 3,4-di-O-caffeoylquinate also potently inhibited thromboxane formation from endogenous arachidonic acid (Chang and Hsu, 1992) and ochnaflavone, also isolated from L. japonica, strongly inhibited rat platelet phospholipase A2 (Chang et al., 1994).
3.1.6. Lian Qiao (Fructus Forsythia)
Lian Qiao (rengyo) is prepared from the dried fruit of Forsythia suspensa Vahl. (Oleaceae). It is used traditionally as an anti-pyretic and an anti-inflammatory agent in the treatment of bacterial infections (Chang and But, 1986; Tang and Eisenbrand, 1992). Water extracts of Fructus Forsythia have been reputed to reduce inflammation and fever in vivo (Chang and But, 1987). Methanol and n-hexane fractions of aqueous extracts of F. suspensa have been shown to have anti-inflammatory effects in vivo (Ozaki et al., 1997). One of the anti-inflammatory constituents of the n-hexane extract was found to be 3b-aceto-20,25- epoxydammarane-24-ol (Ozaki et al., 2000).
3.1.7. Sheng Di Huang (Radix Rehmanniae)
Sheng Di Huang (Chinese foxglove root) is prepared from the root of Rehmannia glutinosa Steud (Scrophulariaceae). Similar to rhino horn, it is classified in TCM as an anti-inflammatory and a ‘blood-cooling’ febrifuge (Hsu et al., 1986). Due to its similarity in TCM functions as rhino horn, when combined with rhino horn in TCM prescriptions, the two remedies are often considered as the most important ingredients (Xu, 1994). However, R. glutinosa is not attributed with the anti-convulsant properties of rhino horn (Xu, 1994). Rehmannia glutinosa has shown potential anti-inflammatory effects through the inhibition of COX (Prieto et al., 2003), TNF-a and IL-1 (Kim et al., 1999) secretion, in vitro.
3.1.8. Xuan Shen (Radix Scrophulariae)
Xuan Shen (figwort root), prepared from the dried roots of Scrophularia ningpoensis Hemsl possesses anti-inflammatory properties and is a ‘blood-cooling’ febrifuge (Hsu et al., 1986; Wiseman and Ye, 1998). Phenylpropanoid glycosides (angoroside C and acteoside) isolated from the root of S. ningpoensis have demonstrated anti-oxidant effects in vitro (Li et al., 2000). Constituent iridoids glycosides (aucubin, verbenalin, and loganin) are reported to show anti-inflammatory effects in vivo (Recio et al., 1994); aucubin has been shown to exert anti-inflammatory activity through the inhibition of the leukotriene, LTC4, in vitro (Bermejo et al., 2000).
3.1.9. Zi Cao (Radix Arnebiae)
Zi Cao (purple gromwell root) is prepared from the root of Arnebia euchroma I.M.Johns+ (Boraginaceae). Like rhino horn, it is classified as a ‘blood cooling’ febrifuge in TCM (Hsu et al., 1986). Arnebia euchroma demonstrated anti-inflammatory activity, in vivo (Kaith et al., 1996) and in vitro through the inhibition of COX-2 activity (Subbaramaiah et al., 2001). Shikonin, a compound isolated from the root of Arnebia euchroma has also been reported to demonstrate anti-inflammatory activity, in vivo and in vitro (Wang et al., 1994; Ko et al., 1995).
3.2. Prescriptions traditionally containing rhino horn: reputed and pharmacological effects
3.2.1. Qing Ying Tang
Qing Ying Tang is a decoction for ‘clearing heat’ in the ‘ying’ system and contains eight herbs in addition to rhino horn (Zhu, 1989; Zou, 1989; Xu, 1994). Rhino horn (Rhinoceros Cornu) and Sheng Di Huang (Radix Rehmanniae) are the two principal (important) remedies and they function by ‘clearing heat’ from the ‘ying’ and blood systems. Other prescription components are described in Table 3.3. The combined horn-herb extracts, and prescription absent from animal product, were anti-pyretic in vivo (But and Tam, 1991).
3.2.2. Qingwen Baidu Yin
The prescription Qingwen Baidu Yin is an anti-pyretic and anti-toxic decoction used to ‘clear away’ heat from ‘qi’ and blood systems (Xu, 1994). The prescription contains 12 herbs, one mineral and rhino horn. Five of the herbs (Sheng Di Huang, Xuan Shen, Lian Qiao, Huang Lian and Dan Zhu Ye) are included in the Qing Ying Tang prescription. The two important components are regarded as rhino horn and Sheng Di Huang. Other prescription components are described in Table 3.3. A modified version of Qingwen Baidu Yin, with buffalo horn substituted for rhino horn, was found to be effective in reducing fever in vivo, but the prescription without added animal product was not tested (Xie, 1993).
3.2.3. Xi Jiao Dihuang Tang
Xi Jiao Dihuang Tang is a prescription used to ‘clear away’ heat from ‘qi’ and blood systems (Zhu, 1989; Bensky and Barolet, 1990; Xu, 1994) It contains rhino horn (the principal component) and three herbs, as described in Table 3.3. All four components of Xi Jiao Dihuang Tang are also included in Qingwen Baidu Yin.
3.2.4. Sheng Xi Dan
Sheng Xi Dan is also known as ‘magical rhinoceros special pill’ (Bensky and Barolet, 1990). It is composed of rhino horn and 10 herbs (Table 3.3.).
3.2.5. Qing Gong Tang
Qing Gong Tang is used in the treatment of epidemic febrile diseases. It is composed of rhino horn and five herbs (Table 3.3.).
3.2.6. Zhi Zi Jin Hua
Zhi Zi Jin Hua is listed in the Pharmacopoeia of the People’s Republic of China (1997) as an anti-pyretic agent and it is composed of eight herbs (Table 3.3.).
3.3. Alternatives to rhino horn: summary
Based on both traditional use and knowledge of the medicinal properties of the different species of plants, a selection of 9 single herbs were chosen for investigation as alternatives to rhino horn in TCM. Six TCM prescriptions were also investigated; five contained rhino horn as the only animal component and one TCM prescription was composed only of herbs. All six prescriptions are used in TCM to treat epidemic febrile diseases. The nine single herbs chosen as possible herbal ‘alternatives’ to rhino horn were found to be included in one or more prescriptions used in this study. This finding confirmed the practice in TCM of combining remedies with similar functions for their additive and synergistic effects. As with the bear bile research, it may be that combinations of the herbs, based on TCM principles, may be more suitable as replacements for animal product use. Rhino horn is used in TCM as a detoxifying, anti-convulsant and anti-inflammatory agent. A major use of rhino horn is in the treatment of advanced stages of fever in the ‘ying’ and blood conformation, complicated by delirium or coma. The herbs and prescriptions selected for investigation were tested in anti-bacterial and anti-inflammatory assays. The methods used and results obtained are reported in Sections 5 and 6 of this report.
4. Rationale for selection of herbs as potential alternatives to tiger bone
4.1. Introduction
This section addresses the selection of potential alternatives to tiger bone in TCM. In terms of finding herbal alternatives to animal products in traditional practices of medicine, the need is perhaps most urgent with that of tiger bone, where hunting has driven the species to the brink of extinction. As with the herbs selected to investigate as potential alternatives for bear bile and rhino horn, selection has been based on investigation of both traditional use and the medicinal properties of the different species of plants and fungi. Sources of tiger bone and the devastating effect of hunting on the tiger population, its uses in TCM and its reported pharmacological activities are discussed. As with the research seeking alternatives to bear bile and rhino horn, both single herbs and prescriptions were selected for investigation. A summary of some of the known constituents and available pharmacological and clinical research on the selected herbs / fungi, and the prescriptions, is given.
4.2. Sources of tiger bone
One of the world’s most endangered animal species is the tiger, Panthera tigris (Felidae). There are only five out of eight remaining subspecies (P. t. amoyensis, P. t. sumatrae, P. t. altaica, P. t. corbetti and P. t. tigris) surviving today, with an estimated population of 5,000 – 7,500 (WWF, 2000). Consequently, P. tigris is included in Appendix 1 of CITES (2003).
In view of the concerns relating to the declining numbers of tigers, investigations were conducted to identify plants or fungi that may be suitable alternatives to tiger bone in TCM. Both TCM principles and pharmacological activities were considered to assist with the identification of suitable species in this study.
4.3. Tiger bone and its constituents
Tiger bone is reported to contain collagen, fats, calcium phosphate, calcium carbonate and magnesium phosphate; the gelatin is reputed to be composed of 17 amino acids (Chang and But, 1987). Generally, bone is primarily composed of inorganic calcium salts (65–70%); smaller amounts of choidroitin sulphate, keratin sulphate and phospholipids are also reported to be present (Brody, 1994). In the UK, choidroitin sulphate is included in some over-the-counter remedies that are used to relieve symptoms of arthritis. There is a general lack of published literature on tiger bone and there is limited evidence to support the pharmacotherapeutic potential of tiger bone for alleviating symptoms of arthritis (Chang and But, 1987). Suspensions of both tiger bone and dog bone are reported to be anti-inflammatory in vivo (Chang and But, 1987); however, the doses used in this study appeared to be much higher than would usually be administered therapeutically. Tiger bone powder is reported to reduce total neutrophil concentration and to inhibit leukocyte and lymphocyte proliferation in vivo (Chang and But, 1987). Both tiger and dog gelatin are reported to be analgesic in vivo (Chang and But, 1987), and tiger and dog bones are reported to be sedative in vivo (Chang and But, 1987). Chang and But (1987) also cite research conducted on a TCM prescription, ‘compound union pill’, containing tiger bone which promoted healing of fractures in rabbits. Analysis of each component of this prescription showed that tiger bone was one of the most effective ingredients to replenish bone density and promote healing (Chang and But, 1987).
4.4. Tiger bone in TCM
Tiger bone (Hu Gu) is described in TCM as having a ‘pungent’ taste and ‘warm’ nature (Chang and But, 1987; Bensky and Gamble, 1993). It is believed to ‘dispel wind-dampness’, ‘disperse wind cold’ and ‘strengthen the sinews and bones’ (Bensky and Gamble, 1993). Tiger bone is used in TCM to treat symptoms such as bone and muscle pain, limb spasms, lower back pain and chills. It is used to treat pathologic states classified under ‘painful obstruction disorders’ in TCM. This group of disorders best fits the Western term ‘arthritic disorders’ which includes various rheumatic diseases and osteoarthritis (Guilaume and Chieu, 1996).
4.5. Selection of herbs
4.5.1. Criteria used for selection of single herbs
There is some limited scientific evidence to support the use of tiger bone as an anti- inflammatory and an analgesic agent in traditional medicine. In order to identify species, which possessed the appropriate TCM properties and functions, an extensive literature survey was initially conducted using the criteria described in Table 4.1. Forty-six species (Table 4.2.) were identified based on the criteria. Although, all the species listed in Table 4.2 may be used in combination with other TCM remedies in the treatment of arthritis and rheumatism, several of them are not categorised as anti-rheumatics in TCM Materia Medicas, and may have other functions (e.g. as a tonic).
| Table 4.1. Properties / functions of tiger bone used as criteria for species selection | |
| Criteria | Properties and functions of tiger bone |
| A | For arthritic and rheumatic conditions |
| B | Analgesic |
| C | ‘Warm’ nature |
| D | ‘Pungent’ or ‘acrid’ |
| E | ‘Sweet’ taste |
| F | Heals wounds and fractures |
| G | Alleviates pain in lower back and knees |
| H | Expels wind dampness or cold |
4.5.2. Criteria used for the selection of prescriptions
In addition to the literature survey conducted to identify appropriate species, another survey was conducted to identify TCM prescriptions that included tiger bone as a component. Those prescriptions identified were generally indicated for arthritis or related disorders. In consultation with TCM practitioners, two TCM prescriptions that contained tiger bone as the only animal component and non-endangered plant / fungal species (those not restricted by CITES) were selected for further investigation (prescription compositions are described in Table 4.3.). The two TCM prescriptions were composed of a combined total of 19 different TCM herbs and one fungus; eight of these species were identified in the initial literature survey of the herbs (Table 4.2.). Since TCM often uses remedies with similar functions to form prescriptions, preliminary pharmacological investigations were conducted to assess the potential anti-inflammatory effects of the two TCM prescriptions; 19 species were also subjected to analysis in the bioassays (Table 4.3. and 4.4.). This approach was designed to identify species used in the prescriptions, which may have anti-inflammatory properties via the biological pathway tested. In addition to the preliminary pharmacological investigations, which were conducted in this study to identify any scientific basis for the reputed activities of the 19 selected remedies,a literature search was also conducted. This aim of this investigation was to identify any pharmacological or clinical studies relating to the potential anti-inflammatory / anti-rheumatic / analgesic effects of the 19 selected remedies (Tables 4.3. and 4.4.). This exercise was to provide information previously reported that might also assist in the identification of possible alternatives to tiger bone. The results of this study are summarised in section 4.6.
| Table 4.2. TCM species identified from evaluation of TCM literature using criteria based on the TCM functions and properties of tiger bone | ||||||||
| TCM herbs | A | B | C | D | E | F | G | H |
| Arthritis Rheumatic | Analgesic | Warm | Pungent (acrid) | Sweet | Wounds & fractures | Lower back & knee pain | Expels wind dampness / cold | |
| 1. Fang Feng, root of Saposhnikovia divaricata
(Turcz.) Schischk. (Apiaceae) |
* | * | * | * | * | * | ||
| 2. Wei Ling Xian, root and rhizome of Clematis chinensis Osb. (Ranunculaceae) | * | * | * | * | * | * | ||
| 3. Nao Yang Hua, aerial part of Rhododendron molle Siebold & Zucc. (Ericaceae) | * | * | * | * | * | * | ||
| 4. Du Huo, root of Angelica pubescens Maxim. (Apiaceae) | * | * | * | * | * | |||
| 5. Fu Zi, prepared daughter root tuber of
Aconitum carmichaelii Debx. (Ranunculaceae) |
* | * | * | * | ||||
| 6. Cang Er Zi, fruit of Xanthium sibiricum Patrin ex Widd. (Asteraceae) | * | * | * | * | * | |||
| 7. Xi Xin, whole plant of Asarum heterotropoides forma manshuricum (Maxim.) Kitag. (Aristolochiaceae)* | * | * | * | * | ||||
| 8. Zu Shi Ma, bark or root bark of Daphne giraldi
Nitsche (Thymelaeaceae) |
* | * | * | * | ||||
| 9. Yang Jin Hua, corolla of Datura metel L. (Solanaceae) | * | * | * | * | ||||
| 10. Chuan Shan Long, rhizome of Dioscorea nipponica Makino (Dioscoreaceae) | * | * | * | * | * | * | ||
| 11. Ba Jiao Feng, leaves, stems and fibrous roots of Alangium chinense (Lour.) Harms (Alangiaceae) | * | * | * | * | ||||
| 12. Qi Ye Lian, roots, stems and leaves of
Schefflera arboricola Hayata (Araliaceae) |
* | * | * | * | ||||
Continued…
| Table 4.2. TCM species identified from evaluation of TCM literature using criteria based on the TCM functions and properties of tiger bone | ||||||||
| TCM herbs | A | B | C | D | E | F | G | H |
| Arthritis Rheumatic | Analgesic | Warm | Pungent (acrid) | Sweet | Wounds & fractures | Lower back & knee pain | Expels wind dampness / cold | |
| 13. Chuan Xiong, rhizome of Ligusticum chuanxiong Hort. (Apiaceae) | * | * | * | * | ||||
| 14. Qing Feng Teng, stem of Sinomenium acutum
Rehd. (Menispermaceae) |
* | * | * | * | ||||
| 15. Xue Shang Yi Zhi Hao, root of Aconitum brachypodum Diels (Ranunculaceae) | * | * | * | |||||
| 16. Qin Jiao, root of Gentiana macrophylla Pall. (Gentianaceae) | * | * | * | * | ||||
| 17. Fang Ji, root of Stephania tetrandra S.Moore (Menispermaceae) | * | * | * | |||||
| 18. Lei Gong Teng, root of Tripterygium wilfordii
Hook.f. (Celastraceae) |
* | * | * | |||||
| 19. Chou Wu Tong, twigs and leaves of Clerodendron trichotonum Thunb. (Verbenaceae) | * | * | * | |||||
| 20. Dang Gui, root of Angelica sinensis (Oliv.) Diels (Apiaceae) | * | * | * | * | ||||
| 21. Ji Xue Teng, root and stem of Spatholobus suberectus Dunn. (Fabaceae) | * | * | * | * | * | |||
| 22. Yin Yang Huo, aerial parts of Epimedium sagittatum Maxim. (Berberidaceae) | * | * | * | * | ||||
| 23. Cang Zhu, rhizome of Atractylodes lancea (Thunb.) DC. or A. chinensis (D.C.) Koidz. (Asteraceae) | * | * | * | * | ||||
| 24. Ding Gong Teng, root and stem of Erycibe obtusifolia Benth. (Convolvulaceae) | * | * | * | * | ||||
Continued
| Table 4.2. TCM species identified from evaluation of TCM literature using criteria based on the TCM functions and properties of tiger bone | ||||||||
| TCM herbs | A | B | C | D | E | F | G | H |
| Arthritis Rheumatic | Analgesic | Warm | Pungent (acrid) | Sweet | Wounds & fractures | Lower back & knee pain | Expels wind dampness / cold | |
| 25. Ci Wu Jia, root and rhizome of Eleutherococcus senticosus (Rupr. & Maxim.) Rupr. (Araliaceae) | * | * | * | |||||
| 26. Yun Xiang Cao, whole plant of Cymbopogon distans (Nees ex Steudel) Will. (Poaceae) | * | * | * | |||||
| 27. Rou Gui, bark of Cinnamomum cassia D.Don (Lauraceae) | * | * | * | |||||
| 28. Tou Gu Cao, whole plant of Impatiens balsamina L. (Balsaminaceae) | * | * | * | * | ||||
| 29. Xu Chang Qing, root and rhizome of Cynanchum paniculatum Bunge (Asclepiadaceae) | * | * | ||||||
| 30. Xue Lian, root of Saussurea laniceps
Hand.-Mazz (Asteraceae) |
* | * | * | |||||
| 31. Xiang Jia Pi, root bark of Periploca sepium
Bunge (Asclepiadaceae) |
* | * | * | |||||
| 32. Lu Xian Cao, whole plant, Pyrola calliantha
Andres and P. decorata Andres (Pyrolaceae) |
* | * | * | |||||
| 33. Yi Ye Qiu, shoot and root of Securinega suffruticosa (Pall.) Rehd. (Phyllanthaceae) | * | * | * | |||||
| 34. Huang Jing Zi, fruit of Vitex negundo L. (Lamiaceae) | * | * | ||||||
| 35. Shi Diao Lan, whole plant of Lysionotus pauciflorus Maxim. (Gesneriaceae) | * | * | ||||||
| 36. Kun Ming Shaun Hai Tang, root of Tripterygium hypoglaucum Hutchinson (Celastraceae) | * | * | ||||||
| 37. Mu Gua, fruit of Chaenomeles speciosa
(Sweet) Nakai (Rosaceae) |
* | * | ||||||
| Table 4.2. TCM species identified from evaluation of TCM literature using criteria based on the TCM functions and properties of tiger bone | ||||||||
| TCM herbs | A | B | C | D | E | F | G | H |
| Arthritis Rheumatic | Analgesic | Warm | Pungent (acrid) | Sweet | Wounds & fractures | Lower back & knee pain | Expels wind dampness / cold | |
| 38. Sang Zhi, young branches of Morus alba L. (Moraceae) | * | * | * | |||||
| 39. Fu Zi, prepared daughter root tuber of
Aconitum carmichaelii Debx. (Ranunculaceae) |
* | * | ||||||
| 40. Nu Zhen Zi, fruit of Ligustrum lucidum Ait. (Oleaceae) | * | * | * | |||||
| 41. Sang Ji Sheng is the stem and branch of
Taxillus chinensis (DC.) Danser (Loranthaceae) |
* | * | * | |||||
| 42. Jin Gi Er, seed of Caragana microphylla Lam. (Leguminosae) | * | * | ||||||
| 43. Man Shan Xiang, Lysimachia capillipes Hemsl. (Primulaceae) | * | * | ||||||
| 44. Qian Cao, root and stem of Rubia cordifolia L. (Rubiaceae) | * | * | ||||||
| 45. Jiu Jie Feng, root, aerial part or whole plant of Sarcandra glabra (Thunberg) Nakai (Chloranthaceae) | * | * | ||||||
| 46. Ma Qian Zi, seed of Strychnos nux-vomica L. (F of China) (Loganiaceae) | * | * | ||||||
References: Chinese Pharmacopoeia, 2005; Chang and But, 1987; Bensky and Gamble, 1993 and 2004; Chang and But, 2001.
| Table 4.3. Composition of herbs as described TCM prescriptions, traditionally containing tiger bone | ||
| Herbs | Yang Xue Gu Feng Tang | Du Huo Ji Sheng Tang |
| Bai Shao, root of Paeonia lactiflora (Ranunculaceae) f | * | * |
| Dang Gui, root of Angelica sinensis (Apiaceae) f | * | * |
| Du Huo, root of Angelica pubescens (Apiaceae) f | * | * |
| Fu Ling, sclerotium of Poria cocos (Polyporaceae) fungus | * | * |
| Niu Xi, root of Achyranthes bidentata (Amaranthaceae) f | * | * |
| Qin Jiao, root of Gentiana macrophylla (Gentianaceae) f | * | * |
| Di Huang, root of Rehmannia glutinosa (Scrophulariaceae) | * | * |
| Bai Zhu, rhizome of Atractylodes macrocephala (Asteraceae) f | * | |
| Gui Zhi, twigs of Cinnamomum cassia (Lauraceae) f | * | |
| Mu Xiang, root of Saussurea costus (Falc.) Lipsch. (Asteraceae) f | * | |
| Sang Chi (Sang zhi), twig of Morus alba (Moraceae) | * | |
| Xu Duan, rhizome of Dipsacus asper (Dipsacaceae) | * | |
| Chuan Xiong, rhizome of Ligusticum chuanxiong (Apiaceae) f | * | |
| Du Zhong, bark of Eucommia ulmoides (Eucommiaceae) f | * | |
| Fang Feng, root of Saposhnikovia divaricata (Apiaceae) f | * | |
| Gan Cao, rhizome of Glycyrrhiza uralensis (Leguminosae) f | * | |
| Ren Shen, root of Panax ginseng (Araliaceae) f | * | |
| Rou Gui, bark of Cinnamomum cassia (Lauraceae) | * | |
| Sang Ji Sheng, stem and branch of Taxillus chinensis (Loranthaceae) f | * | |
f Species also tested individually in biological activity tests
| Table 4.4. Other species selected for biological activity tests (not listed in Table 4.3.) |
| Herbs |
| Cang Zhu, rhizome of Atractylodes lancea+ (Asteraceae) |
| Mu Gua, fruit of Chaenomeles speciosa (Rosaceae) |
| Wei Lin Xian, root and rhizome of Clematis chinensis (Ranunculaceae) |
| Yin Yang Huo, aerial parts of Epimedium sagittatum (Berberidaceae) |
| San Qi, root of Panax pseudoginseng (Araliaceae) |
+ Other plant species may be used for the Chinese name specified (not listed in Table 4.4.)
4.6. Single herbs and other TCM remedies as potential alternatives to tiger bone:reputed and pharmacological effects
4.6.1. Bai Shao (Radix Paeoniae Alba)
Bai Shao is the dried root of Paeonia lactiflora Pall (Ranunculaceae) and is used to treat a variety of disorders in TCM including spasmodic pain of the limbs; Paeonia root may also be used for analgesic effects (Pharmacopoeia of PRC, 2000; Tang and Eisenbrand, 1992). Few studies have been conducted to investigate the anti-inflammatory potential of P. lactiflora, however, it has been associated with activity against COX (Prieto et al., 2003). Paeoniflorin, isolated from the root, is reported to be anti-inflammatory (Tang and Eisenbrand, 1992).
4.6.2. Bai Zhu (Rhizoma Atractylodis Macrocephalae)
Bai Zhu is the dried rhizome of Atractylodes macrocephala Koidz. (Asteraceae) and it is indicated in TCM for a number of disorders, which include oedema (Tang and Eisenbrand, 1992; Pharmacopoeia of PRC, 2000). Limited research has been conducted to investigate the anti-inflammatory potential of A. macrocephala, but it has been associated with activity against COX (Prieto et al., 2003).
4.6.3. Cang Zhu (Rhizoma Atractylodis)
Cang Zhu is the dried rhizome of Atractylodes lancea DC. or A. chinensis Koidz (Asteraceae) and it has been used in TCM for the treatment of rheumatic arthralgia (Pharmacopoeia of PRC, 2000). Some compounds (including phenols, polyacetylenes, atractylon (sesquiterpene) and osthole (coumarin)) from A. lancea rhizomes and lipophilic extracts have been associated with inhibition of COX-1 and 5-LOX (Resch et al., 1998; Resch et al., 2001). A Japanese prescription used traditionally for arthritis treatment and composed of seven crude drugs including A. lancea was anti-inflammatory in vivo (Kimura et al., 1991). Pharmacological studies regarding A. chinensis are lacking.
4.6.4. Chuan Xiong (Rhizoma Chuanxiong)
Chuan Xiong is the dried rhizome of Ligusticum chuanxiong Hort. (Apiaceae), which is used in TCM for various conditions such as rheumatic arthralgia (Tang and Eisenbrand, 1992; Pharmacopoeia of PRC, 2000). There is a relative lack of research regarding the pharmacological basis of the reputed anti-inflammatory / anti-rheumatic activity of
- chuanxiong. An alcohol extract is reported as anti-inflammatory and analgesic (Chang and But, 2001). Tetramethylpyrazine, an alkaloid from L. chuanxiong, has been associated with anti-inflammatory activity in both the early and late stages of inflammation (Ozaki, 1992).
4.6.5. Dang Gui (Radix Angelicae Sinensis)
Dang Gui is prepared from the dried root of Angelica sinensis (Oliv.) Diels (Apiaceae) and it is indicated in TCM for a number of disorders including rheumatic arthralgia and traumatic injuries (Tang and Eisenbrand, 1992; Pharmacopoeia of PRC, 2000). There is a relative lack of research regarding the pharmacological basis of the reputed anti-inflammatory / anti- rheumatic activity of A. sinensis. Ferulic acid, reported to occur in A. sinensis, has been associated with anti-inflammatory activity in both the early and late stages of inflammation (Ozaki, 1992).
4.6.6. Di Huang (Radix Rehmanniae)
Di Huang is the fresh or dried root tuber of Rehmannia glutinosa Steud. (Scrophulariaceae) and is used in TCM to treat various disorders and may be used as a tonic (processed roots) or haemostatic (fresh and dried roots) (Tang and Eisenbrand, 1992; Pharmacopoeia of PRC, 2000). An extract (100% methanol) of R. glutinosa root showed inhibition of COX-2 and iNOS activity (Hong et al., 2002). An aqueous extract of R. glutinosa root has been suggested to inhibit TNF-a secretion by inhibiting IL-1 secretion and R. glutinosa root extract may have anti-inflammatory activity in the CNS (Kim et al., 1999). However, in vivo, an ethanolic extract of R. glutinosa root was ineffective on the development of oedema in arthritic rats and on chronic and acute inflammation (Kubo et al., 1994). It is also reported that it is only the decoction which has an anti-inflammatory effect and not an alcohol extract (Chang and But, 2001).
4.6.7. Du Huo (Radix Angelicae Pubescentis)
Du Huo is the dried root of Angelica pubescens Maxim. (Umbelliferae), which has been used in TCM as an analgesic and anti-rheumatic agent (Tang and Eisenbrand, 1992; Pharmacopoeia of PRC, 2000). Anti-inflammatory and analgesic activities of A. pubescens root are well documented (Chen et al., 1995; Kosuge et al., 1985; Liu et al., 1998a; Liu et al., 1998b; Prieto et al., 2003). Methanol, chloroform and ethyl acetate extracts are reported to reduce pain and oedema in vivo; columbianadin, columbianetin acetate, bergapten, umbelliferone and caffeic acid were anti-inflammatory and analgesic in vivo; osthole and xanthotoxin were anti-inflammatory in vivo (Chen et al., 1995). A. pubescens, A. pubescens f. biserrata, linoleic acid, osthole, osthenol and some polyacetylenes (e.g. falcarindiol) have also been associated with inhibition of COX and 5-LOX (Liu et al., 1998a; Liu et al., 1998b). 1.pubescens is also reported to be effective in attenuating persistent hindpaw inflammation and hyperalgesia in rats (Wei et al., 1999).
4.6.8. Du Zhong (Cortex Eucommiae)
Du Zhong is the dried stem bark of Eucommia ulmoides Oliver (Eucommiaceae) and is reputed in TCM to strengthen the tendons and bones (Tang and Eisenbrand, 1992; Pharmacopoeia of PRC, 2000). The chemical composition of E. ulmoides has been subjected to some investigation and pharmacological activities have been associated with some constituents. However, there is a comparative lack of research regarding pharmacological studies associated with anti-inflammatory or anti-rheumatic activities. A decoction is reported to be analgesic and anti-inflammatory (which may be related to enhancement of adrenocortical function) in vivo (Chang and But, 2001).
4.6.9. Fang Feng (Radix Saposhnikoviae)
Fang Feng is the dried root of Saposhnikovia divaricata (Turcz.) Schischk. (Apiaceae) and it is used in TCM to treat rheumatic arthralgia (Pharmacopoeia of PRC, 2000). The ethanol extract of Fang Feng is reported to be analgesic and anti-inflammatory (Chang and But, 2001). Analgesic components of S. divaricata are reported to be chromones, coumarins, polyacetylenes and 1-acylglycerols; the most potent analgesia was associated with chromones such as divaricatol, ledebouriellol and hamaudol (Okuyama et al., 2001). Imperatorin and deltoin, isolated from S. divaricata root, inhibited the expression of the iNOS protein (Wang et al., 1999).
4.6.10. Fu Ling (Poria)
Fu Ling is the dried sclerotium of the fungus Poria cocos (Polyporaceae), which is indicated in TCM for a number of disorders and is reputed to cause diuresis and to calm the mind (Pharmacopoeia of PRC, 2000). P. cocos is reported to inhibit 5-LOX and phospholipase
A2 activities and dehydrotumulosic and pachymic acids, which have been isolated from
- cocos, are reported to inhibit leukotriene B4 (LTB4) release and to inhibit phospholipase A2 activity (Cuellar et al., 1996; Giner et al., 2000; Giner-Larza et al., 2000; Prieto et al., 2003). A triterpene derivative (3b-p-hydroxybenzoyldehydrotumulosic acid) isolated from
- cocos showed anti-inflammatory activity in vivo (Yasukawa et al., 1998).
4.6.11. Gui Zhi (Ramulus Cinnamomi)
Gui Zhi is the dried young branches of Cinnamomum cassia (Lauraceae), which has been used in TCM for the treatment of arthralgia and oedema (Tang and Eisenbrand, 1992; Pharmacopoeia of PRC, 2000). An extract (100% methanol) of C. cassia twigs showed inhibition of COX-2 and iNOS activity (Hong et al., 2002), which may explain some of the reputed effects. The active constituents responsible for activities observed in pharmacological studies require further investigation.
4.6.12. Ji Xue Teng (Caulis Spatholobi)
Ji Xue Teng is the root and stem of Spatholobus suberectus Dunn (Fabaceae) and it has been used in TCM for various conditions, which include knee pain or generalised joint soreness (Bensky and Gamble, 1993). Ji Xue Teng is reported to promote beneficial effects on artificially-induced arthritis in vivo (Bensky and Gamble, 1993). In addition, the alternative plant species used to prepare Ji Xue Teng, S. suberectus stem, was active against COX-1, phospholipase A2, 5-LOX and 12-LOX activities, but did not inhibit COX-2 activity (Li et al., 2003).
4.6.13. Lu Lu Tong (Fructus Liquidambaris)
Lu Lu Tong is the dried ripe fruit of Liquidambar formosana Hance (Hamamelidaceae) and it is indicated for arthralgia with numbness and muscular contracture (Pharmacopoeia of PRC, 2000). Some studies have investigated the chemistry of Liquidambar species, however, pharmacological studies are limited; anti-inflammatory / anti-rheumatic effects have not been substantially investigated.
4.6.14. Mu Gua (Fructus Chaenomelis)
Mu Gua is the dried nearly ripe fruit of Chaenomeles speciosa Nakai (Rosaceae) and it is indicated in TCM for arthritis with ankylosis (Pharmacopoeia of PRC, 2000). Glucosides from C. speciosa were anti-inflammatory (effects included inhibition of TNF-a and PGE2) in vivo (Chen and Wei, 2003; Dai et al., 2003).
4.6.15. Mu Xiang (Radix Aucklandiae)
Mu Xiang is the dried root of Saussurea costus (Falc.) Lipsch (Syn.: Saussurea lappa) (Asteraceae) and it is used in TCM for treating some types of pain (Pharmacopoeia of PRC, 2000). An ethanolic extract of S. lappa is reported to show anti-inflammatory and anti- arthritic activity (Gokhale et al., 2002). Sesquiterpene lactones (e.g. costunolide, cynaropicrin) from Saussurea lappa have been associated with anti-inflammatory activity (Cho et al., 2000; Gokhale et al., 2003; Matsuda et al., 2003; Cho et al., 2004). The anti-inflammatory activity of the sesquiterpene lactone fraction of S. lappa has been suggested to be due to stabilisation of lysosomal membranes and an anti-proliferative effect (Gokhale et al., 2003). Cynaropicrin inhibited TNF-a release, attenuated nitric oxide accumulation and dose- dependently suppressed the proliferation of lymphocytes (Cho et al., 2000); costunolide inhibited IL-1b gene expression (Kang et al., 2004). Some amino acid-sesquiterpene conjugates (saussureamines A and B) from a methanolic extract of S. lappa roots inhibited activation of NF-kB (Matsuda et al., 2003).
4.6.16. Niu Xi (Radix Achyranthis Bidentatae)
Niu Xi is prepared from the dried root of Achyranthes bidentata Blume (Amaranthaceae) and is used in TCM as a tonic and for soreness of the lumbar and knee joints with weakness in the legs (Tang and Eisenbrand, 1992; Pharmacopoeia of PRC, 2000). There is a general lack of research regarding the study of potential anti-inflammatory / anti-rheumatic effects of A. bidentata. An oligosaccharide (AbPS) isolated from A. bidentata significantly enhanced the humoral immune response and antagonised the immunosuppressive effects of cyclosporin A; AbPS increased the production of TNF and the activity of natural killer cells; in tumour patients treated by chemotherapy or radiotherapy, AbPS maintained their peripheral white blood cell count and improved the quality of life (Li, 2000). Root polysaccharides induced IL-1 and TNF-a synthesis and secretion from mouse peritoneal macrophages in vitro, indicating immunopotentiating activity (Xiang and Li, 1993).
Leflunomide (disease modifying anti-rheumatic drug in clinical use) and its active metabolite are associated with inhibition of IL-1b, TNF-a and NF–kB (Breedveld and Dayer, 2000; Elkayam et al., 2003), thus A. bidentata saccharides may be of no therapeutic benefit in rheumatoid arthritis (RA) via these mechanisms (in view of the reported association with immunopotentiating effects).
4.6.17. Qin Jiao (Radix Gentianae Macrophyllae)
Qin Jiao is the dried root of Gentiana macrophylla Pall. It has been used in TCM mainly for the treatment of rheumatic or rheumatoid arthritis with muscular contracture and severe joint pain (Tang and Eisenbrand, 1992; Pharmacopoeia of PRC, 2000). Compounds identified in Gentiana macrophylla include various secoiridoids. The secoiridoid glucoside, gentiopicroside, is reported to show anti-inflammatory activity in vivo (Tang and Eisenbrand, 1992).
4.6.18. Ren Shen (Radix Ginseng)
Ren Shen is the dried root of Panax ginseng C.A.Mey (Araliaceae) and it is indicated for various conditions, including general weakness with irritability and insomnia in chronic diseases, and may be included in prescriptions as a tonic (Tang and Eisenbrand, 1992; Pharmacopoeia of PRC, 2000). P. ginseng has been extensively researched regarding its chemistry and its pharmacological and clinical effects. Ginsenoside Rg3 inhibited COX-2 expression and NF–kB activation (Keum et al., 2003).
4.6.19. Rou Gui (Cortex Cinnamomi)
Rou Gui is the dried stem bark of Cinnamomum cassia D.Don (Lauraceae), which was used traditionally for cold and pain in the knees and for some inflammatory disorders (Tang and Eisenbrand, 1992; Pharmacopoeia of PRC, 2000). An extract (70% methanol) of C. cassia cortex showed an inhibitory effect on acute inflammation in vivo (Kubo et al., 1996). Further investigation is required to identify the active constituents responsible for these effects.
4.6.20. San Qi (Radix Notoginseng)
San Qi is the dried root of Panax notoginseng (Burkill) Chen (Araliaceae), which is used in TCM to alleviate traumatic swelling and pain, amongst other conditions (Pharmacopoeia of PRC, 2000; Tang and Eisenbrand, 1992). Saponins from Panax notoginseng are reported to be anti-inflammatory, which may be associated with inhibition of phospholipase A2 activity (Hao and Yang, 1986; Tang and Eisenbrand, 1992; Li and Chu, 1999). Another study showed that P. notoginseng did not produce any significant effect on inflammation and hyperalgesia in vivo (Wei et al., 1999).
4.6.21. Sang Zhi (Ramulus Mori)
Sang Zhi is the dried young branches of Morus alba L. (Moraceae) and is used for the treatment of arthritis and rheumatism (Tang and Eisenbrand, 1992; Pharmacopoeia of PRC, 2000). An extract (100% methanol) of M. alba twigs showed inhibition of iNOS activity (Hong et al., 2002). Mulberroside A and oxyresveratrol, obtained from M. alba cortex, have been investigated for their anti-inflammatory activity and were shown to significantly reduce paw oedema (Chung et al., 2003). The anti-inflammatory properties of oxyresveratrol were associated with inhibition of NOS expression through down-regulation of NF–kB binding and inhibition of COX-2 activity (Chung et al., 2003).
4.6.22. Wei Ling Xian (Radix Clematidis)
Wei Ling Xian is the dried root and rhizome of Clematis chinensis Osb. (Ranunculaceae), and it is indicated in TCM for rheumatic or rheumatoid arthralgia with numbness of the limbs (Tang and Eisenbrand, 1992; Pharmacopoeia of PRC, 2000). Stems of C. chinensis have also been used in TCM to treat rheumatic arthritis and other inflammatory conditions (Xu et al., 1996). In one study, an ethanol extract of C. chinensis stems only inhibited COX- 1 activity in vitro at high concentrations (Li et al., 2003). Few pharmacological studies have been conducted to investigate any scientific basis for the reputed anti-inflammatory / anti- rheumatic effects of C. chinensis.
4.6.23. Xu Duan (Dipsaci Radix)
Xu Duan is the dried root of Dipsacus asperoides C.Y.Cheng & T.M.Ai (Dipsacaceae), which is indicated in TCM for aching and weakness of the loins and knees, rheumatic arthralgia and traumatic injuries (Pharmacopoeia of PRC, 2000). D. asperoides has not been subjected to substantial investigation regarding its chemistry and pharmacological activities.
4.6.24. Yin Yang Huo (Herba Epimedii)
Yin Yang Huo is prepared from the dried aerial parts of Epimedium sagittatum (S. et Z) Maxim (Berberidaceae); it is indicated in TCM for weakness of the limbs and rheumatic or rheumatoid arthralgia with numbness or muscle contracture, and has also been included in prescriptions as a tonic (Tang and Eisenbrand, 1992; Pharmacopoeia of PRC, 2000). A flavonoid extract from E. sagittatum was effective in preventing osteoporosis in vivo, which may be mediated by enhancement of osteoblast development (Chen et al., 2004). Other studies, relating to the potential anti-inflammatory / anti-rheumatic effects of the species used to prepare Yin Yang Huo are limited, and further investigations are necessary to establish the basis for their clinical use.
4.7. Alternatives to tiger bone: summary
Based on both traditional uses and evidence from scientific research, a selection of 19 single herbs and 2 prescriptions (Tables 4.3. and 4.4.) were selected. Five other species present in some TCM prescriptions also traditionally containing tiger bone, were chosen for further study (Table 4.4.). In TCM, tiger bone is traditionally used to treat conditions involving inflammation and this property is supported by research suggesting that suspensions of both tiger bone and dog bone are anti-inflammatory in vivo. Preliminary pharmacological investigations were therefore conducted to assess the potential anti-inflammatory effects of the selected herbs and prescriptions. The methods used are reported in Section 5 of this report and the findings are reported in Section 6. This approach was designed to identify species used in the prescriptions, which may have anti-inflammatory properties via the biological pathway tested.
5. Biological and chemical methods used to study plant and fungal material
5.1. Introduction
Both rhino horn and bear bile are primarily classified in TCM as anti-inflammatory and fever-reducing remedies and tiger bone has been used as an anti-arthritic / anti-rheumatic remedy (Hsu et al., 1986); the pathology of arthritis also involves inflammatory mechanisms. Thus, assays were selected to evaluate the anti-inflammatory potential of the TCM material. The inflammatory response is a complex cascade of events, often triggered by infection (commonly by bacteria) and is one of the body’s defence mechanisms in fighting disease. The inflammatory response forms one of the underlying pathologies of arthritis (McEvoy, 2004); fever (Ivanov and Romanovsky 2004); liver diseases (Tanasescu, 2004), cancer (Ross et al., 2004) and cardiovascular diseases (Brown and Jones, 2004). Therefore, preliminary studies were conducted to assess the effects of crude extracts, fractions and isolated compounds on bacterial growth and an anti-inflammatory mediator, nuclear factor-kappaB (NF-kB), in vitro. NF-kB is a transcriptional factor which regulates the genes of several pro-inflammatory chemicals, such as cytokines (IL-1b, IL-6, IL-8, TNF-a), enzymes (COX-2, iNOS), adhesion molecules and in a self-regulatory way its inhibitory protein, I-kB (Bremner and Heinrich, 2002; Ross et al., 2004). CYP3A4 inhibition tests, using testosterone 6b-hydroxylation as a probe for enzyme activity, were conducted in human liver microsomes, to determine the effect of herbal extracts on drug metabolising enzyme in vitro. In this study, TCM material was extracted using solvents of varying polarity and the resulting extracts were tested in a range of bioassays. Preliminary studies were conducted using aqueous extracts since this extraction procedure reflects the preparation of decoctions in TCM. Prior to testing in the bioassays, the chemical profiles of the plant material, obtained from commercial companies, were compared with the chemical profiles of authentic and other reference material, obtained from the Chinese Medicinal Plant Authentication Centre (CMPAC), Royal Botanic Gardens, Kew. Verification of the TCM material is essential to ensure that, when interpreting data regarding the chemistry and pharmacological activities of each species, the results refer to the correct species. This is of particular concern, as TCM material may be adulterated or deliberately substituted with other plant species. A TCM name for a herb may refer to more than one plant species, for example Chi Shao is prepared from the dried root of Paeonia lactiflora or Paeonia veitchii. Thus, when recommending potential alternatives to the animal material (bear bile, rhino horn, tiger bone), it is essential to ensure the correct species is being proposed as an alternative. This process involved comparison of the chemical profiles of the commercial material with verified TCM material (available from the collections held at CMPAC, Royal Botanic Gardens, Kew) using various chromatographic techniques. Some other concerns associated with the use of traditional herbal medicines (in particular TCM) are the safety of the remedies (Koh and Woh, 2000). Therefore, in addition, it was important to determine if the herbs contained high levels of pesticide residues (Appendix 2) and heavy metals (Appendix 3).
5.2. Materials
Many of the samples of the TCM material were kindly donated by Jo Liu of Mayway (UK) Ltd. (Hanwell, UK) and Paul Skipworth of Kingham Herbs and Tinctures (UK). Rhino horn was kindly donated by the CITES team (Special Operations District, Heathrow airport) and tiger bone (obtained from the rib of a male hybrid Amur tiger), was donated by the National Museums of Scotland. Ursodeoxycholic acid (UDCA) was purchased from Sigma chemicals (UK). Authentic and other reference (market) samples of TCM material, used to assist with authentication of the trade TCM material, were obtained from CMPAC, Royal Botanic Gardens, Kew.
5.3. Authentication techniques for trade TCM material
TCM material (trade samples and reference material) was ground using a pestle and mortar or grinding equipment, to provide sufficient material for authentication procedures and bioassays. Ground material was then extracted using aqueous 80% methanol, and as different types of compounds were targeted to assist with the authentication process, the ground material of some species was also extracted using other solvents (water, ethanol, dichloromethane or hexane). Following extraction, extracts were filtered, evaporated to dryness (aqueous extracts were freeze-dried) and reconstituted in the appropriate solvent, prior to HPLC and LC-MS analysis.
5.3.1. HPLC (UV-DAD) method
Analytical HPLC was carried out using a Waters LC600 pump and a 996 photodiode array detector. A Merck LiChrospher 100RP-18 (250 x 4.0 mm i.d. 5 µm particle size) column (maintained at 30°C) was used for analysis with a flow rate of 1 ml/min. The mobile phase consisted of 2% aqueous acetic acid (A) and methanol : acetic acid : water (18:1:1). Initial conditions were 75% A and 25% B; the proportion of B increased with a linear gradient, reaching 100% at t = 20 min. This was followed by an isocratic elution of 100% B until t = 25 min. Injections (30 µl) were made by an autosampler.
5.3.2. LC-MS method
LC-MS analysis was conducted at the Royal Botanic Gardens, Kew, by Dr G. Kite. Aqueous 80% methanol extracts were analysed using a Thermo-Finnigan LC/MS/MS system consisting of a ‘Surveyor’ autosampling LC system, interfaced to a ‘LCQ Classic’ quadrupole ion trap mass spectrometer. Chromatographic separation of compounds was performed on a 250 mm x 4.6 mm i.d., 5 µm Supelco Discovery-C18 column using a 1 ml/min mobile phase gradient programmed from water (A), methanol (B) and methanol containing 5% acetic acid (C). The gradient programme (A:B:C) was 80:0:20 (t = 0 min), 0:80:20 (t = 20 min), 0:80:20 (t = 25 min), 80:0:20 (t = 27 min), 80:0:20 (t = 37 min). Data analysis was performed using Xcalibur 1.2 software (Thermo-Finnigan).
5.3.3. TD-GC-MS method
The TD-GC-MS system used consisted of a Perkin-Elmer ATD400 thermal desorption unit, a Perkin-Elmer AutoSystem XL GC and a Perkin-Elmer TurboMass MS (quadrupole). Chromatography was performed on a 30 m x 0.25 mm i.d. x 0.25 µm DB-5MS column (J. & W. Scientific, USA) using an oven program of 60–300°C at 6°C/min. The carrier gas was helium at a flow rate of 1 ml/min. The TCM material was analysed using desorption; the inlet split flow was 0 ml/min and the outlet split flow was 18.75 ml/min, the desorption flow was 60 ml/min, the desorption temperature was 150°C, the trap temperature was 4°C and the pressure was 14.6 psi. Detection was by mass-spectrometry; the MS was fitted with an EI source operated at 70eV with a source temperature of 180°C, and mass spectra were recorded in the range m/z 38–300. The software was Turbomass, version 4.1.1. Approximately 2 mg of dried TCM material was desorbed for each analysis. Compounds were identified by comparing mass spectra with published data (Ausloss et al., 1992; Adams, 2001).
5.4. Methods for fractionation and isolation of compounds
- Fractionations of Scutellaria baicalensis and isolation of compounds
Dried powdered root of S. baicalensis (35 g) was extracted in MeOH (800 ml) using a Soxhlet apparatus for 19 h (64°C). The extract was concentrated to about 300 ml and partitioned using hexane (100 ml). Column chromatography using normal phase silica gel (60A S-230/70 mesh, SL06SA4, YMC Co. Ltd) was conducted on the dried methanol layer (12 g). The mobile phase used was a step gradient elution of 10 combinations (each 500 ml) of CHCl3, Me2CO, MeOH and H2O in increasing polarity, starting with 100% CHCl3 and ending with 95% MeOH in H2O. A total of 20 fractions were collected and concentrated separately to dryness. HPLC-(UV-DAD) analysis, anti-bacterial and anti inflammatory (NF-kB) tests were conducted on the crude extracts of S. baicalensis and each of the 20 fractions. Fraction 4 (SB4) was selected for further fractionation based on the results obtained from NF-kB tests. Preparative TLC was adopted as a method to fractionate SB4 using a mobile phase of hexane: CHCl3: EtOAc (1:1:1). Nine fractions were obtained and tested in anti-bacterial and anti-inflammatory (NF-kB) assays. The fifth fraction of SB4 (SB4v) demonstrated potent NF-kB inhibition. Therefore SB4v was fractionated using preparative HPLC-UV-DAD and NMR spectroscopy was used to identify the compounds isolated. NMR data were acquired and interpreted at the Royal Botanic Gardens, Kew, by Dr N. Veitch.
- Fractionation of Salvia miltiorrhiza and Qing Ying Tang
Dried powdered root of S. miltiorrhiza (72 g) was extracted in MeOH (800 ml) by using a Soxhlet apparatus for 17 h (64°C). The extract was concentrated to dryness and 11 g was subjected to silica column chromatography. A gradient elution of 8 combinations of CHCl3, MeOH and H2O in increasing polarity, starting with 100% CHCl3 and ending with 85% MeOH in H2O, was employed. A total of 17 fractions were collected. Lypophilised crude hot water extract of the TCM prescription, Qing Ying Tang (2.4 g) was fractionated using flash chromatography (reversed-phase). A stepwise gradient elution system was used starting with 5% MeOH in water and ending with 100% MeOH in volumes of 600 ml each. Twenty-four fractions were collected. Anti-bacterial tests were performed on the fractions obtained from which S. miltiorrhiza and Qing Ying Tang. The fractions which showed some anti-bacterial activity were tested in an anti-inflammatory (NF-kB) assay.
5.5. Method for anti-bacterial tests
Assays were conducted at the Royal Botanic Gardens, Kew with Dr T. Kokubun. The method for assessing anti-bacterial activity was a modification of that described by Rehalison et al. (1991). For this study, 20 µl aliquots of each herb extract (5 mg/ml) or fraction (1 mg/ml) were applied to three replicate TLC plates (20 x 10 cm2, pre-coated aluminium-backed silica gel, 60F254 sheets, Merck, Germany). The TLC plates were developed in a tank containing one of the following solvent systems: chloroform : acetone (4:1) or (17:3), or chloroform : acetone : water (7:3:1). Developed plates were observed under UV light (254 nm and 355 nm). One TLC plate was subjected to chemical analysis and two were used to conduct anti-bacterial tests. The TLC plate for chemical analysis was sprayed evenly with p-anisaldehyde (0.5 ml in 50 ml HOAc and 1 ml conc. H2SO4); the chemical profile of the sprayed plate was examined under UV light (355 nm). After heating, plates were re-examined under UV light (355 nm). Two of the developed TLC plates were fixed onto separate culture dishes and chloramphenical (3 µg/ml; positive control) was applied to a solvent-free area on each TLC plate. A small colony of previously cultured bacteria (Pseudomonas syringae, ID No. IMI347448, CABI Bioscience, UK or Bacillus subtilis, ID No. IMI347329, CABI Bioscience, UK) was suspended in water and added to 50 ml nutrient agar solution to form a seeded medium. This medium was used as an overlay on the TLC plate to form bioautograms with a layer of approx 1 mm thickness of medium. The bioautographs were sealed and incubated overnight (37°C, 100 % relative humidity). After incubation the bioautographs were stained with p-iodonitrotetradium violet (2-[4-indophenyl]-3-[4-nitrophenyl]-5-phenyltetrazolium chloride, Sigma, USA) diluted in ethanol (0.5 mg/ml, diluted 10-fold immediately prior to use). The dishes were incubated (at 37°C) for a further two hours and then visually examined. Areas on the plate with inhibited or reduced bacterial growth appeared as white spots against a pink background. Areas of inhibition were compared to corresponding areas in the chemically treated plates to ascertain groups of compounds responsible for the inhibition of bacterial growth.
5.6. NF–kB studies using the IL-6 promoter assay method
Dr P. Bremner conducted the assays as part of the collaboration with Professor M. Heinrich, School of Pharmacy, London. The assay used was as described by Bork et al. (1999). HeLa S3 cells were stably transfected with IL-6 promoter fused with a Luciferase reporter gene for 24 hours. Extracts/fractions (final incubation concentration of 100 µg/ml in DMSO) and compounds (prepared in acetone) were placed in 96-well plates and incubated with the transfected cells (at 37°C; 95% humidity) for 1 hour. The cells were then stimulated with 50 ng/ml (final concentration) of either phorbol myristate acetate (PMA, Sigma, UK) or TNF-a (Sigma, UK) and incubated for a minimum of 7 hours (maximum 14 hours) before harvesting. To each well, 100 µl of lysis buffer (25 mM Tris-phosphate pH 7.8, 8 mM MgCl2, 1 mM DTT, 1% Triton X-100 and 7% glycerol) was added and left for 15 minutes. After harvesting the cells, beetle Luciferin (50 µl, Promega, USA) was added to the lysed cells (15 µl) in a 96-well plate by an automated Luminoter/photometer (Anthos Lucy 1, Rosys Anthos, Switzerland) and the light emission was measured following a reaction time of 10 seconds. The light emission of the lysis buffer was obtained as a background reading and subtracted from each experimental value. Positive controls consisted of cells stimulated with either PMA or TNF-a only and negative controls involved cells subjected to no stimulation.
5.7. Method for cytochrome P450 3A4 inhibition studies
A Tecan Genesis 150 RSP (Tecan UK Ltd, Reading, UK) was used to incubate the test solutions in 96-well plates using an automated set-up and timed procedures. The following sequence was performed, in duplicate, by the RSP. Ketoconazole (0.1, 0.3, 1, 3 and 10 µM), herbal extracts and fractions (1000 µg/ml in water), compounds (200 µg/ml in 2.5% acetone) and negative controls (water or 2.5% acetone) were placed in 96-well plates. Phosphate buffer (0.1 M; 245 µl) was added to human liver microsomes containing testosterone (100 nM; 50 µl). A test solution (50 µl) was then added. The plates were pre-incubated for 2 minutes. NADPH regenerating mixture (155 µl) was added to each tube (to give a final volume of 0.5 ml) and incubated at 37 +– 2°C for 20 minutes. Phosphoric acid (0.15 M; 0.1 ml) was added to terminate the reactions.
Instrumental quality control samples were performed (for each 96-well plate) by preparing tubes containing the human liver microsomes (50 µl) (with no added testosterone) and phosphate buffer (0.1 M; 245 µl). After the 2 minutes pre-incubation, NADPH mixture (155 µl) was added to each tube (to a final volume of 0.45 ml) and incubated as described above. On the termination of the reactions, by the addition of phosphoric acid, 6b-hydroxytestosterone (50 µl; 10 and 100 µM) was used to generate duplicate quality samples at two concentrations (1 µM and 10 µM). All the incubation tubes were centrifuged at 3000 rpm for 10 minutes at ambient temperature. Aliquots of each sample were placed in HPLC vials using the RSP. The incubation procedure described above resulted in a 10 times dilution of the test solutions. Therefore, the herbal extracts and compounds were tested at final concentrations of 100 µg/ml and 20 µg/ml, respectively. Baicalin (45 µM), baicalein (74 µM), scutellarein (69 µM) and chrysin (79 µM) were tested. The final concentrations for ketoconazole were 0.01, 0.03, 0.1, 0.3 and 1 µM.
5.7.1. CYP3A4 LC-MS method
Liquid chromatographic-mass spectrometric (LC-MS) analysis was conducted using a 1100 HPLC system (Agilent, Berks., UK) interfaced with mass spectrometer. The chromatographic determination of 6b-hydroxytestosterone was performed on a 150 mm x 4.6 mm i.d., 5 µm Luna Phenyl Hexyl column (Phenomenex, Cheshire, UK) with a sentry 20 mm x 2.9 mm Symmetry C8 guard cartridge (Waters, Mass., USA) at 25°C. A flow rate of 1.5 ml/min was used with mobile phase gradient programmed between ammonium acetate buffer (A) and acetonitrile (B). The gradient programme (A:B) was 81:19 (t = 0); 73:27 (t = 3 minutes); 10:90 (t = 10 min) and then back to the original mobile phase ratio of 81:19 at t = 11 minutes till t = 11.5 minutes. The injection volume was 50 µl. The MS detection was made in the positive ion mode, with TurboIonspray, 500°C, flow split 1:5. The nebuliser gas was set at 8 (arbitrary scale), auxiliary gas at 6 L/min, and the curtain gas was set at 10 L/min. The ionspray voltage was 4800 mV, orifice voltage (declustering potential) was 31 mV, ring voltage (focussing potential) was 180 mV and the Q0 voltage (entrance potential) was -5 mV. The ion was monitored at m/z = 305.6 with a scan time of 500 ms. Data were acquired for 10 minutes per sample. The approximate retention time for 6b-hydroxytestosterone was 8.5 minutes.
5.8. Statistical analysis
The values obtained for the NF-kB and CYP450 assays were expressed as mean values +– SD. The Student’s 1-sample t-test was used to determine statistical differences between test and control groups. The difference was considered statistically significant when p < 0.05.
6. Results and discussion
6.1. Bear bile: bioassay results and discussion
Results of the authentication study indicate that at least five of the seven TCM herbs (Table 6.1.) showed similar chemical profiles to the reference and authentic material, thus indicating they were the correct plant species, as described in TCM.
| Table 6.1. TCM herbs for which the plant species were identified |
| Chuan Xin Lian, aerial part of Andrographis paniculata (CXL) |
| Zhi Mu, rhizome of Anemarrhena asphodeloides (ZM) |
| Zhi Zi, fruit of Gardenia jasminoides (ZZ) |
| Huang Qin, root of Scutellaria baicalensis (SB) |
| Huang Bai, cortex of Phellodendron amurense (HB) |
| TCM herbs for which the plant species were not verified |
| Huang Lian, Rhizoma Coptidis (HL)* |
| Da Huang, Radix et Rhizoma Rhei (DH)* |
6.1.1. Anti-bacterial tests
The seven herbs described in Table 6.1., as well as prescription X were tested for their effect on Gram-positive and Gram-negative bacteria. Some components from ethyl acetate extracts (100 µg) of the following six herbs, separated on TLC plates, showed inhibitory action against the growth of Bacillus subtilis (Gram-positive bacteria): Anemarrhena asphodeloides, Gardenia jasminoides, Scutellaria baicalensis, Phellodendron amurense, Coptis chinensis and Rheum palmatum. In addition, some fractions from the ethyl acetate extract (100 µg) of Rheum palmatum and fractions from the methanol extract (20 µg) of Scutellaria baicalensis also inhibited the growth of Pseudomonas syringae (Gram-positive bacteria). Out of the seven herbs tested only Andrographis paniculata showed no inhibitory effect against either Bacillus subtilis or Pseudomonas syringae at 100 µg. However, some TCM literature cites studies conducted in China, which have shown that Andrographis paniculata inhibits several Gram-negative and Gram-positive bacteria in vitro, but the concentrations tested were not stated (Hsu et al., 1986; Chang and But, 1987; Huang, 1999). Prescription X (100 µg) did not inhibit either Bacillus subtilis or Pseudomonas syringae at the concentration tested.
6.1.2. Anti-inflammatory (NF-kB) tests
Herbal extracts (100 µg/ml) were tested in either TNF-a or PMA-stimulated HeLa cells using an IL-6 promoter method to determine their effect on NF–kB activity; results are shown in Fig. 6.1. Water extracts of Rheum palmatum (DH) showed significant (p<0.05) inhibition of NF–kB activity. Water extracts of Coptis chinensis (HL), Phellodendron amurense (HB) and Anemarrhena asphodeloides (ZM) reduced NF–kB activity; however, these reductions were not statistically significant. A water extract of Andrographis panicalata (CXL) did not affect NF–kB production. Also, prescription X reduced Luciferase values by 16%, but this was not statistically significant (data not shown).
Although potent inhibition of NF–kB activity was measured for the ethyl acetate extract of Scutellaria baicalensis (69%, p<0.001), stimulation was obtained for the corresponding water, methanol (SBM) and hexane (SBH) extracts (Fig. 6.1.). The effects of fractions (SB1 – SB20; obtained from methanol extract) of S. baicalensis on NF–kB activity are shown in Fig 6.2.
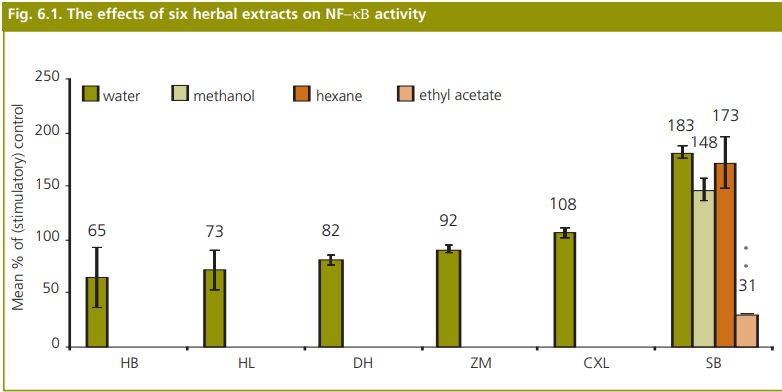
Fig. 6.1. The effects of six herbal extracts on NF−κΒ activity
Cells for water extracts (100 µg/ml) were stimulated with phorbol myristate acetate (PMA; 50 ng/ml) and the ethyl acetate extract (100 µg/ml) with TNF-a (50 µg/ml). Induced IL-6 promoter activity was measured as light emission (Luciferase values) expressed as a percentage relative to cells stimulated by PMA or TNF-a only. The data represent mean (n = 3) ± SD. *p<0.05 and **p<0.001 indicate statistically significant differences from cells treated with PMA or TNF-a only. Codes for herbs presented in Fig. 6.1: HB: Huang bai, cortex of Phellodendron amurense; HL: Huang lian, Rhizoma Coptidis ; DH: Da Huang, Radix et Rhizoma Rhei; ZM: Zhi Mu, rhizome of Anemarrhena asphodeloides; CXL: Chuan Xin Lian, aerial part of Andrographis paniculata; SB: Huang Qin, root of Scutellaria baicalensis.
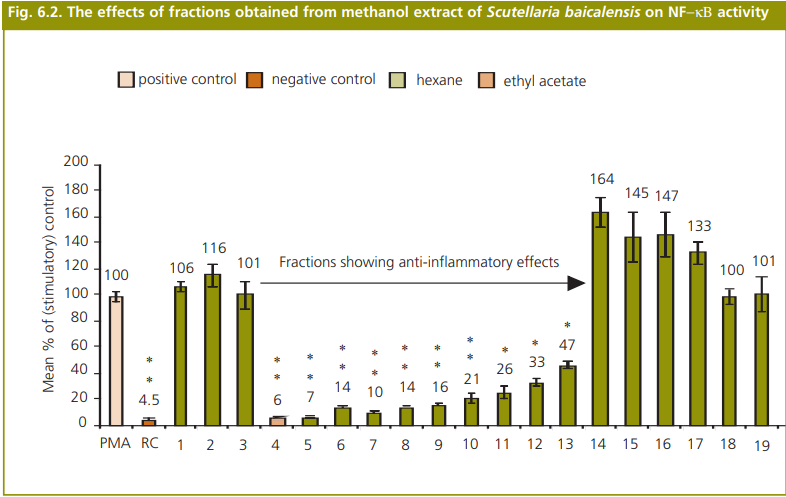
Fig. 6.2. The effects of fractions obtained from methanol extract of Scutellaria baicalensis on NF−κΒ activity
Extracts (100 µg/ml) were tested in PMA-stimulated cells. IL-6 gene promoter activity was measured as outlined in the legend for Fig. 6.1. Negative controls: resting cells (RC; unstimulated); positive controls: PMA stimulated cells. The data represent mean (n = 9 for controls and n = 3 for test samples) ± SD. *p= 0.001, **p<0.001 indicate statistically significant differences from PMA-stimulated cells. Colour code: yellow = positive control (stimulatory); red = resting cells (inhibitory); purple = other fractions obtained from fractionating the crude extract; orange = fraction further fractionated. Fraction 4v (obtained from fractionating fraction 4) = 3%, p<0.001.
Fractions SB4-SB13 demonstrated significant inhibition of NF-kB activity (p< 0.001), in contrast to the stimulatory effects of some fractions (SB14-SB17) and the crude methanolic extract (SBM). Three compounds, chrysin, wogonin and oroxylin A, were isolated and identified from SB4 using TLC, HPLC (UV-DAD) and NMR. These three flavonoids were also identified from their characteristic UV profiles, as present in active fractions SB4 to SB12 from HPLC-(UV-DAD) analysis. When the constituents of S. baicalensis (chrysin, wogonin, oroxylin A, baicalein, baicalin and scutellarein) were tested, the NF-kB inhibitory and stimulatory activities of some of these compounds were found to be dependent on their concentrations (Fig. 6.3). Salicylic acid, an anti-inflammatory compound, which inhibits COX activity, was used as a further control in this assay. Chrysin inhibited NF-kB activity in a dose-dependant manner (at 50–393 µM, p<0.001), showing more inhibitory activity than salicylic acid (145 µM, p<0.01; Fig 6.3). Baicalein and wogonin demonstrated a significant reduction in NF-kB activity, only at 370 and 100 µM, respectively. However, chrysin and baicalein had some associated cytotoxity at 393 µM and 370 µM, respectively.
At lower concentrations chrysin (25 µM) and wogonin (25 and 50 µM) demonstrated significant stimulation of NF-kB activity (Fig. 6.3.). Oroxylin A also stimulated NF-kB activity at 25–100 µM (p<0.05) but showed no significant effect at 352 µM. However, oroxylin A (70 µM) has been reported to inhibit LPS-induced NF-kB activity in RAW264.7 macrophages via the inhibition of NF-kB complex (Chen et al., 2000). The anti-inflammatory pathway tested in the current study was via the inhibition of NF-kB activity (as assessed using IL-6 promoter assay). Recently, baicalein (24, 48 and 96 µM) has been reported to potently inhibit IL-12 production in LPS-activated macrophages via the inhibition of NF-kB binding activity (Kang et al., 2003a).
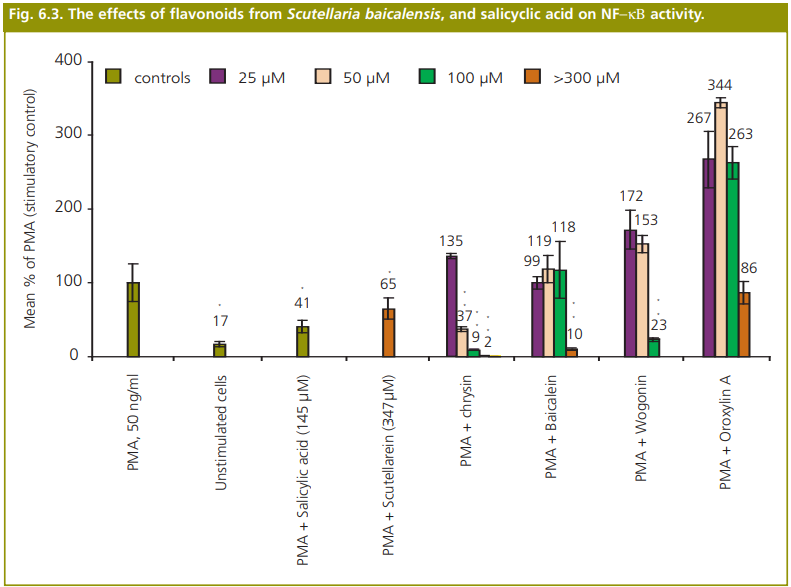
Fig. 6.3. The effects of flavonoids from Scutellaria baicalensis, and salicyclic acid on NF−κΒ activity. Compounds were tested in PMA-stimulated cells; IL-6 promoter activity was measured as outlined in the legend for Fig.6.1. The data represent mean (n = 8 for PMA, n = 9 for resting cells and n = 3 for test compounds) ± SD. *p<0.01, **p<0.001 indicate statistically significant differences from PMA-stimulated cells. Scutellarein (5,6,7,4’- tetrahydroxyflavone); baicalin (5,6-dihydroxy-7-glucuronide); chrysin (5,7-dihydroxyflavone); baicalein (5,6,7- trihydroxyflavone); wogonin (5,7-dihydroxy-8-methoxyflavone); oroxylin A (5,7-dihydroxy-6-methoxyflavone).
6.1.1. Cytochrome P450 3A4 tests
Results for the CYP3A4 inhibition assay, using testosterone 6b-hydroxylation as a probe for enzyme activity in human liver microsomes, are presented in Figs 6.4 and 6.5. Crude hot water extracts of Coptis chinensis (100 µg/ml) significantly reduced CYP3A4 activity by 37% (p <0.01) compared to that of the negative (uninhibited) control (Fig. 6.4). Water extracts of Scutellaria baicalensis, Anemarrhena asphodeloides, Andrographis paniculata, Phellodendron amurense and Gardenia jasminoides showed no significant effect CYP3A4 activity at 100 µg/ml (Fig. 6.4).
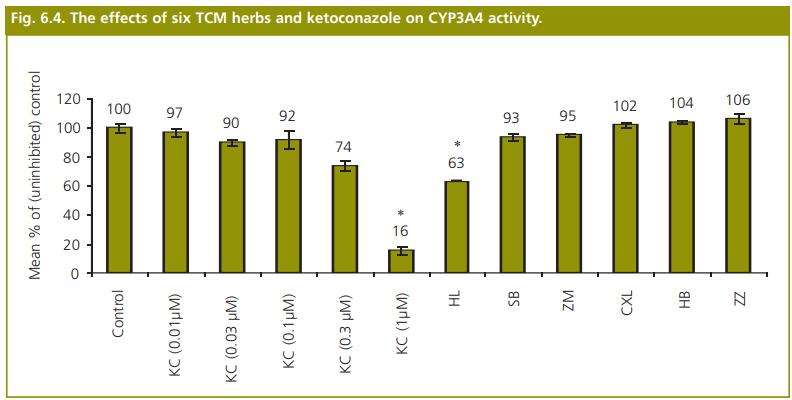
Fig. 6.4. The effects of six TCM herbs and ketoconazole on CYP3A4 activity. The assay was conducted using testosterone 6β-hydroxylation as a probe for enzyme activity in human liver microsomes.
Results were calculated as mean % of uninhibited controls (water); ketoconazole (KC) was used as positive control. Data represent mean (n = 2) ± SD. *p<0.01 indicate statistically significant differences from groups only treated with water. Codes for herbs presented in Fig. 6.4: HL: Huang lian, Coptis chinensis; Huang qin, root of Scutellaria baicalensis; ZM: Zhi Mu, rhizome of Anemarrhena asphodeloides; CXL: Chuan Xin Lian, aerial part of Andrographis paniculata; SB: HB: Huang Bai, cortex of Phellodendron amurense; ZZ: Zhi Zi, fruit of Gardenia jasminoides.
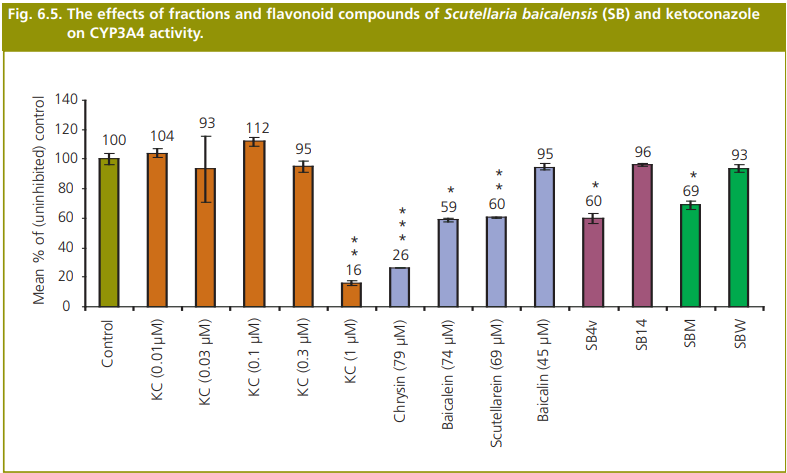
Fig. 6.5. The effects of fractions and flavonoid compounds of Scutellaria baicalensis (SB) and ketoconazole on CYP3A4 activity. The assay was conducted using testosterone 6β-hydroxylation as a probe for enzyme activity in human liver microsomes. Results were calculated as mean % of uninhibited controls (water); ketoconazole (KC) was used as positive control. Data represent mean (n = 2) + SD. *p<0.05, **p<0.01, ***p<0.001 indicate statistically significant differences from groups only treated with water. Colour codes: red = unstimulated controls (water or 2.5% acetone); yellow = ketoconazole; blue = known compounds of S. baicalensis; plum = fractions obtained from fractionating S. baicalensis; green = crude extracts of S. baicalensis.
However, a methanolic extract of Scutellaria baicalensis (SBM), a fraction (SB4v) and two constituent flavonoids, baicalein (74 µM) and scutellarein (69 µM), from Scutellaria baicalensis all inhibited CYP3A4 activity by 30–40 % (p<0.05) compared to the negative (uninhibited) control (Fig. 6.5). Chrysin (79 µM), showed greater inhibition by lowering CYP3A4 activity to 74% (p<0.001) compared to the negative (uninhibited) control (Fig.
6.5). The IC50 value obtained for the positive control, ketoconazole in the CYP3A4 studies was 0.6 µM, which was high, compared to reported values of 0.1 µM (McKillop et al., 1999) and 0.04 mM (Sai et al., 2000). The high positive control value observed may indicate that moderate inhibition might not have been detected with some of the
test extracts at the concentration tested.
6.1.1. Conclusions
Results from this study have shown that Anemarrhena asphodeloides, Gardenia jasminoides, Scutellaria baicalensis, Phellodendron amurense, Rhizoma Coptidis and Radix et Rhizoma Rhei all possess some anti-bacterial activity. Also, results from this study have further confirmed the anti-inflammatory properties of Radix et Rhizoma Rhei and Scutellaria baicalensis through the inhibition NF-kB activity. The results from both the anti-bacterial and anti-inflammatory tests have highlighted the herbs which may be investigated further through bioactivity guided fractionations.Preliminary results from the CYP3A4 studies suggest that possible herb-herb interactions may occur in preparations containing both Rhizoma Coptidis and Scutellaria baicalensis (such as Dia-Orengedokuto and Orengedokuto). Also, drug-herb interactions may occur when herbal preparations containing Rhizoma Coptidis and/or Scutellaria baicalensis are co-administered with some pharmaceutical drugs, which are metabolised by CYP3A4. However, further work is required to investigate the extent of these effects.
6.2. Rhino horn: bioassay results and discussion
Twenty-two herbs that could be potential substitutes for rhino horn were assayed for activity (Table 6.2). The extracts of the 22 herbs were chemically profiled along with authenticated TCM material. At least 13 of these herbs showed similar chemical profiles to the authenticated TCM samples, thus indicating they were the correct plant species, as described in TCM. Further work is necessary on 9 of the plant species to confirm their identification.
6.2.1. Anti-bacterial tests
Results for anti-bacterial activity of extracts (100 µg) of rhino horn and TCM prescriptions are summarised in Table 6.3. In addition, 24 fractions were obtained from flash chromatography of water extracts of Qing Ying Tang; fractions QYT9, QYT15, QYT16 and QYT17 showed some inhibitory activity against Bacillus subtilis but did not inhibit Pseudomonas syringae. The anti-bacterial tests were qualitative, so although some prescriptions with and without rhino horn demonstrated anti-bacterial activity, the contribution of the horn extracts in the prescriptions could not be evaluated. However, rhino horn alone did not inhibit the growth of either Bacillus subtilis or Pseudomonas syringae. Crude ethyl acetate extracts (100 µg) of Radix et Rhizoma Rhei and fractions from methanolic extracts (20 µg) of Salvia miltiorrhiza, Scutellaria baicalensis and Lonicera japonica showed anti-bacterial activity against both Bacillus subtilis and Pseudomonas syringae. Ethyl acetate extracts (100 µg) of 17 herbs showed some inhibitory activity against Bacillus subtilis and are listed in Table 6.2 (samples 4–20).
| Table 6.2. TCM herbs investigated in biological assays | |
| Abbreviation | TCM herbs |
| MDP | Mu Dan Pi, root of Paeonia suffruticosa |
| JG | Jie Geng, root of Platycodon grandiflorum |
| GC | Gan Cao, root of Glycyrrhiza uralensis |
| XS | Xuan Shen, root of Scrophularia ningpoensis |
| SDH | Sheng Di Huang, root of Rehmannia glutinosa |
| JYH | Jin Yin Hua, flower bud of Lonicera japonica |
| LQ | Lian Qiao, fruit of Forsythia suspensa |
| DS | Dan Shen, root of Salvia miltiorrhiza |
| DZY | Dan Zhu Ye, aerial part of Lophatherum gracile |
| ZM (B) | Zhi Mu, rhizome of Anemarrhena asphodeloides |
| ZZ (B) | Zhi Zi, fruit of Gardenia jasminoides |
| HQ (B) | Huang Qin, root of Scutellaria baicalensis |
| HB (B) | Huang Bai, cortex of Phellodendron amurense |
| Abbreviation | TCM herbs |
| HL (B) | Huang Lian, Rhizoma Coptidis |
| DH (B) | Da Huang, Radix et Rhizoma Rhei |
| ZC | Zi Cao, Radix Arnebiae |
| BLG | Ban Lan Gen, Radix Isatidis |
| MMD | Mai Men Dong, Ophiopogonis Radix |
| DDC | Dan Dou Chi, Semen Sojae Praeparatum |
| CP | Chang Pu, Rhizoma Acori Graminei |
| CSY | Chi Shao, Radix Paeoniae Rubra |
| THF | Tian Hua Fen, Radix Trichosanthis |
(B) Results have also been presented in the bear bile project (section 6.1).
TCM pharmaceutical names are used in the text for herbs that require further investigation to assist with their authentication.
| Table 6.3. Anti-bacterial activity of rhino horn and TCM prescriptions | ||
| Rhino horn and TCM prescriptions | Anti-bacterial tests | |
| B. subtilis | P. syringae | |
| Rhino horn | nd | nd |
| Qing Ying Tang plus rhino horn (QYT + RH) | Inhibition | nd |
| Qing Ying Tang without rhino horn (QYT) | Inhibition | nd |
| Sheng Xi Dan plus rhino horn (SXD+RH) | Inhibition | Inhibition |
| Sheng Xi Dan without rhino horn (SXD) | Inhibition | Inhibition |
| Qing Gong Tang plus rhino horn (QGT+RH) | Inhibition | nd |
| Qing Gong Tang without rhino horn (QGT) | Inhibition | Inhibition |
| Qingwen Baidu Yin plus rhino horn (QWBY + RH) | nd | nd |
| Qingwen Baidu Yin without rhino horn (QWBY) | nd | nd |
| Xi Jiao Dihuang Tang plus rhino horn (XJDHT + RH) | nd | nd |
| Xi Jiao Dihuang Tang without rhino horn (XJDHT) | nd | nd |
| Zhi Zi Jin Hua (ZZJH) | nd | nd |
nd: no inhibition detected
6.2.2. Anti-inflammatory (NF-kB) tests
Water extracts (100 µg/ml) of five TCM prescriptions containing rhino horn and five without rhino horn, rhino horn alone, as well as Zhi Zi Jin Hua (composed only of herbs) were tested in PMA-stimulated HeLa cells using IL-6 promoter assay (Fig 6.6). Only the prescriptions Xi Jiao Dihuang Tang without rhino horn (XJDHT) and Xi Jiao Dihuang tang with rhino horn (XJDHT+RH) showed significant inhibitory effect on NF-kB activity (Fig 6.6.). XJDHT+RH and XJDHT reduced NF-kB activity by 45 % (p<0.01) and 34 % (p<0.05), respectively, compared to fully stimulated cells by PMA, indicating that rhino horn might contribute to the inhibitory effect. However, since rhino horn extract alone did not show any apparent effect on the NF-kB activity and results from the other prescriptions were not conclusive, further work is required to clarify the contribution of the horn extract and whether there is a synergistic effect. The TCM prescription Qing Ying Tang (QYT) demonstrated stimulatory effect on NF-kB activity (Fig. 6.6.). However, when fractions obtained from QYT (QYT9, QYT15, QYT16 and QYT17), that showed anti-bacterial activity were tested in the NF-kB assay they demonstrated significant inhibition of NF-kB activity (Fig. 6.7(A)).
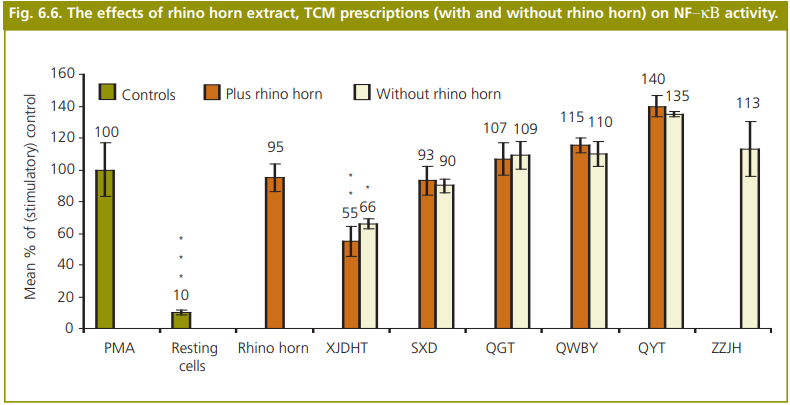
Fig. 6.6. The effects of rhino horn extract, TCM prescriptions (with and without rhino horn) on NF−κΒ activity. Water extracts (100 µg/ml) were tested in PMA-stimulated cells as outlined in Fig. 6.1. Resting cells were used as negative controls; cells stimulated with PMA alone were used as positive controls. The data represent mean (n = 5 for controls and n = 3 for test samples) ± SD. *p<0.05, **p<0.01, ***p<0.001 indicate statistically significant differences from groups only treated with PMA. The abbreviations for the prescriptions are described in Table 6.3.
Salvia miltiorrhiza is one of eight herbs making up the QYT prescription. Fractions SM6 and SM7 from the methanolic extract of Salvia miltiorrhiza potently inhibited NF-kB activity to below levels obtained for resting cells, and SM8 reduced NF-kB activity to 52% of that of PMA (fully stimulated cells) (Fig. 6.7.(A)).
Crude hot water extracts of some of the 16 herbs (found in some of the TCM prescriptions investigated in this study) were also tested in PMA-stimulated HeLa cells in NF-kB tests and the results are presented in Fig. 6.7(B). Paeonia suffruticosa and Radix Trichosanthis significantly reduced NF-kB activity by about 50% of that obtained by cells fully stimulated with PMA. Other herbs showing statistically significant reduction in NF-kB activity were Lophatherum gracile, Radix Isatidis, Rhizoma Coptidis, Semen Sojae Praeparatum and Rehmannia glutinosa (Fig 6.7.(B)).
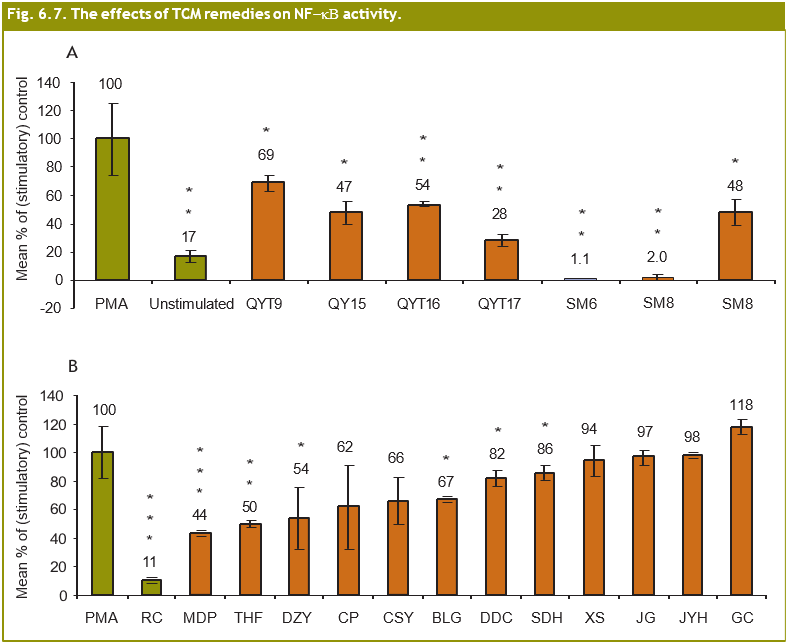
Fig. 6.7. The effects of TCM remedies on NF−κΒ activity.
(A) The effects of fractions (SM6, SM7 and SM8) of a methanol extract of Salvia miltiorrhiza (SM) and water extract of
Qing Ying Tang (QYT).
(B) The effects of 12 TCM herbs (full names are described in Table 6.2).
Extracts (100 µg/ml) were tested in PMA-stimulated cells as outlined in Fig. 6.1. Resting cells (RC) were used as negative
controls; cells stimulated with PMA alone were used as positive controls. The induced IL-6 promoter activity was
measured as light emission (Luciferase values) and expressed as a percentage relative to cells stimulated with PMA
alone. The data represent mean (n = 5 for controls and n = 3 for test samples) ± SD. *p<0.05, **p<0.01,
***p<0.001 indicate statistically significant differences from groups only treated with PMA.
6.2.3. Cytochrome P450 3A4 tests
Water extracts (100 µg/ml) of rhino horn and TCM prescriptions Sheng Xi Dan and Qing Ying Tang (with and without rhino horn) showed no apparent significant effect on 6b-testosterone hydroxylation due to inhibition of CYP3A4 activity (Fig. 6.8. (A)). The IC50 value obtained for the positive control, ketoconazole, in these studies was 0.5 µM. Water extracts (100 µg/ml) of 14 herbs were also tested and only Rhizoma Coptidis and Rehmannia glutinosa showed any significant effect on CYP3A4 activity compared to the control (containing no inhibitor) (Fig. 6.8.(B)). Fraction SM7 obtained from a methanolic extract of Salvia miltiorrhiza also demonstrated inhibitory activity against CYP3A4 activity compared to the control (Fig. 6.8. (C)). The inhibitory effects of some Scutellaria constituents are discussed under the bear bile project (section 6.1.).
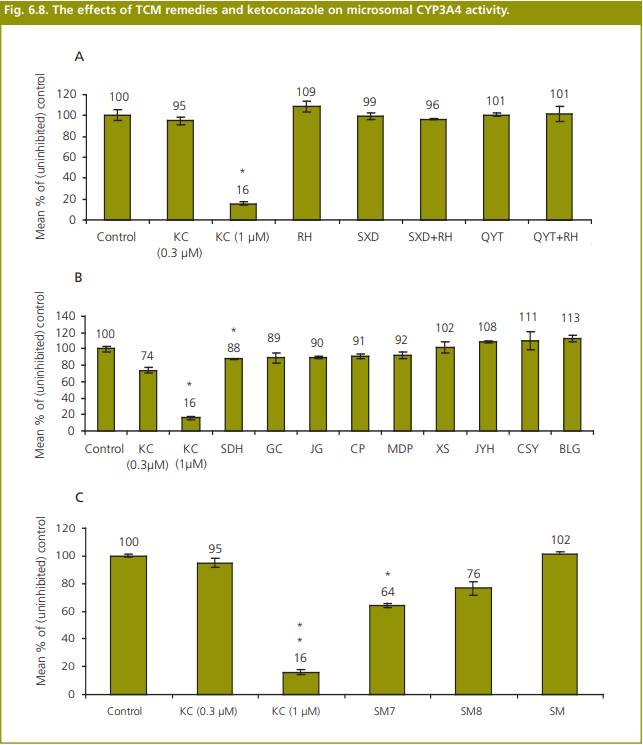
Fig. 6.8. The effects of TCM remedies and ketoconazole on microsomal CYP3A4 activity
A. Rhino horn (RH) and Shen Xi Dan (SXD) and Qing Ying Tang (GYT) with and without
B. Nine TCM herbs (full names are described in Table 2.).
C. Fractions (SM7 & SM8) of a methanol extract of Salvia miltiorrhiza (SM).
The CYP3A4 inhibition assay was conducted using testosterone 6b-hydroxylation as a probe for enzyme activity in human liver microsomes. Results were calculated as mean percent of uninhibited control (water); ketoconazole (KC) was used as positive control. The data represent mean (n = 2) ± SD. *p<0.05, **p<0.01 indicate statistically significant differences from groups only treated with vehicle solution.
6.2.4. Conclusions
Water extracts of rhino horn did not demonstrate anti-bacterial or anti-inflammatory properties, nor did they have any effect on the drug metabolising enzyme, CYP3A4. However, some TCM prescriptions with and without rhino horn showed some anti-bacterial and anti-inflammatory properties in the assays used in this study. However, further work using other bioassays is required to ascertain the contribution of the horn extracts to any activities of the TCM prescriptions. Most of the herbs (17 out of 22) showed some anti-bacterial activity against Bacillus subtilis, indicating potential pharmacological effects. Also, results from this study indicate potential anti-inflammatory properties of four out of the nine herbs selected to study as possible alternatives to rhino horn: Paeonia suffruticosa, Radix Isatidis, Rehmannia glutinosa and Salvia miltiorrhiza. In addition Radix Trichosanthis, Semen Sojae Praeparatum, Rhizoma Coptidis and Lophatherum graciIe, found in different prescriptions also showed anti- inflammatory properties. To date no scientific literature in the English language has been obtained for the anti-inflammatory effects of Lophatherum gracile and therefore further studies are required to verify the data obtained from this study. The TCM prescriptions Xi Jiao Dihuang Tang and Qing Ying Tang also showed a significant anti-inflammatory effect through the inhibition of NF-kB activity. Salvia miltiorrhiza, Rehmannia glutinosa, as well as Scutellaria baicalensis and Rhizoma Coptidis, showed inhibitory effects on CYP3A4 during preliminary studies. Since they are commonly used TCM herbs, further work may be required to determine potential adverse interactions with other remedies.
6.3. Tiger bone: bioassay results and discussion
The extracts of the twenty-three herbs and one fungus were chemically profiled along with authenticated TCM material, using various analytical techniques (HPLC (UV-DAD), LC-MS and GC-MS). At least 10 of the species showed similar chemical profiles to the authenticated TCM samples, thus indicating they were the correct species, as described in TCM. Further analysis of the remaining TCM material is necessary to confirm their identification. Eighteen of the herbs were investigated in biological assays for the tiger bone project (Table 6.4.).
| Table 6.4. TCM samples studied in biological assays | |
| TCM samples studied in biological assays | |
| Tiger bone | Panthera tigris |
| DH(b) | Du Huo, root of Angelica pubescens |
| WLX (a) | Wei Lin Xian, root of Clematis chinensis |
| BS (a) | Bai Shao, root of Paeonia lactiflora |
| YYH (a) | Ying Yang Huo, aerial part of Epimedium sagittatum |
| FF (a) | Fang Feng, root of Saposhnikovia divaricata |
| DZ (a) | Du Zhong, bark of Eucommia ulmoides |
| MX | Mu Xiang, root of Saussurea costus |
| CZ | Cang Zhu, root of Atractylodes lancea |
| RS | Ren Shen, root of Panax ginseng |
| SQ | San Qi, root of Panax pseudoginseng |
| BZ | Bai Zhu, roots of Atractylodes macrocephala |
| SJS | Sang Ji Sheng, stem and branch of Taxillus chinensis |
| CX | Chuan Xiong, rhizome of Ligusticum chuanxiong |
| QJ | Qin Jiao, leaf of Gentiana macrophylla |
| DQ | Dang Gui, root of Angelica sinensis |
| GZ | Gui Zhi, twigs of Cinnamomum cassia |
| NX | Niu Xi, root of Achyranthes bidentata |
| MG | Mu Gua, fruit of Chaenomeles speciosa |
(a) Herbs tested in NF–kB assay only; (b) Herbs tested CYP3A4 assay only
6.3.1. Anti-inflammatory (NF-kB) tests
Crude hot water extracts (100 µg/ml) of tiger bone and the prescription Yang Xue Gu Feng Tang (without tiger bone) reduced NF-kB activity (via the inhibition of IL-6 promoter activity) by 31% and 34%, respectively (p<0.05), in PMA-stimulated HeLa cells (Fig. 6.9(A)). However, the reduction of NF-kB activity (26%) by the prescription, Du Huo Ji Sheng Tang (without tiger bone) was not statistically significant (Fig. 6.9(A)). Results for crude hot water extracts (100 µg/ml) of 17 herbs are shown in Fig 6.9(B). Four of these herbs produced a statistically significant reduction in NF-kB activity: Atractylodes macrocephala (Bai Zhu), Saussurea costus (Mu Xiang), Taxillus chinensis (Sang Ji Sheng) and Angelica sinensis (Dang Qui).
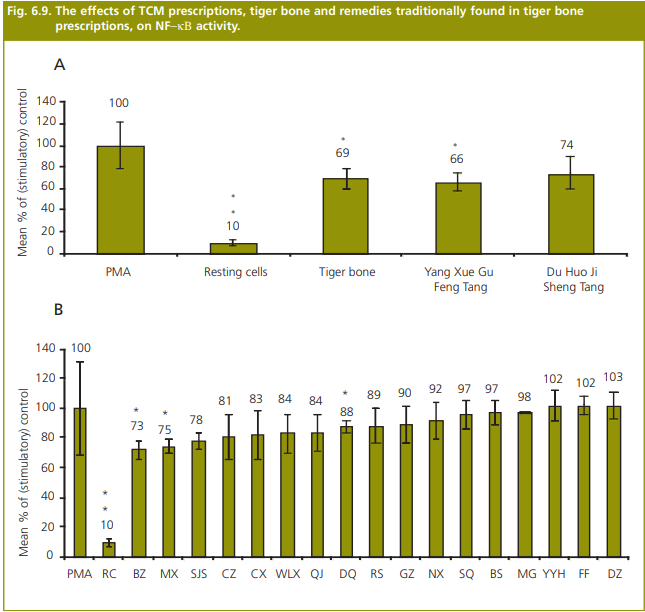
Fig. 6.9. The effects of TCM prescriptions, tiger bone and remedies traditionally found in tiger bone prescriptions, on NF−κΒ activity.
(A) The effects of tiger bone and two TCM prescriptions on NF-kB
(B)The effects of 17 herbs on NF-kB activity (full names are described in Table 4.).
Extracts (100 µg/ml) were tested in PMA-stimulated cells as outlined in Fig. 6.1. The full names of the herbs are as described in Table 6.4. Resting cells (RC; unstimulated) were used as negative controls; cells stimulated with PMA were used as positive controls. The induced IL-6 promoter activity was measured as light emission (Luciferase values) and expressed as a percentage relative to cells stimulated by PMA only. The data represent mean (n = 7 for controls and n = 3 for test samples) + SD. *p<0.05 and **p<0.01 indicate statistically significant differences from groups only treated with PMA.
Although, the inhibitory effects of the herbs were not potent at the concentrations tested, the results have highlighted the herbs that could be investigated further, using other assays to assess potential pharmacological mechanisms that could be related to anti-inflammatory activity.
6.3.2. Cytochrome P450 3A4 tests
Crude hot water extracts (100 µg/ml) of tiger bone and thirteen individual herbs were tested for their inhibitory potential on the metabolising enzyme CYP3A4. Results for the CYP3A4 inhibition assay using testosterone 6b-hydroxylation as a probe for enzyme activity in human liver microsomes is presented in Fig. 6.10. None of the extracts tested showed any apparent significant effect on 6b-testosterone hydroxylation due to inhibition of CYP3A4 activity. These results suggest that tiger bone and the herbs tested may not be modulators of CYP3A4. However, there has been some reported evidence to suggest that some TCM herbs such as Angelica dahurica is an inhibitor of CYP3A4, which was demonstrated by the longer pre-incubation time of the microsomal assay (Guo et al., 2001). Also, the IC50 value obtained for the positive control, ketoconazole in this study was 0.5 µM, which was high compared to reported values of 0.1 µM (McKillop et al., 1999) and 0.04 mM (Sai et al., 2000); and therefore moderate inhibitors may not have been detected.
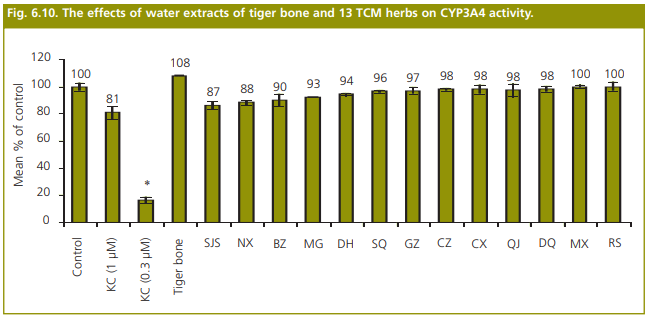
Fig. 6.10. The effects of water extracts of tiger bone and 13 TCM herbs on CYP3A4 activity. e CYP3A4 inhibition assay was conducted using testosterone 6b-hydroxylation as a probe for enzyme activity in human liver microsomes. Results were calculated as mean % of uninhibited control (water); ketoconazole (KC) was used as positive control of inhibition. The data represent mean (n = 2) ± SD. *p<0.01 indicate statistically significant differences from groups only treated with water. The full names of the herbs are described in Table 6.4.
6.3.3. Conclusions
Tiger bone may possess some anti-inflammatory properties, through the inhibition of IL-6 promoter activity. However, further tests are required to confirm this activity. The following 3 herbs (not restricted by CITES, 2004) contained in some existing TCM prescriptions that included tiger bone, showed some potential anti-inflammatory activity: Atractylodes macrocephala (Bai Zhu), Taxillus chinensis (Sang Ji Sheng), and Angelica sinensis (Dang Qui). Although the inhibitory effects of the herbs were not potent at the concentrations tested, the results have highlighted the herbs which could be investigated further. None of the herbs investigated had any effect on CYP3A4; since TCM remedies are sometimes co-administered with pharmaceutical drugs, there is a need for further investigation to determine if the herbs affect different CYP enzymes by different mechanisms.
7. Conclusions
7.1. General conclusions
Following consultation with TCM practitioners to identify potential TCM prescriptions and herbs, consideration of the TCM uses of the plants and their reported pharmacological activities in the literature were used as criteria to select the herbs that could have potential as alternatives to bear bile, rhino horn and tiger bone. Most of the suggested herbal ‘alternatives’ to the animal products are listed as ingredients in one or more TCM prescriptions which traditionally contained the animal products. This finding confirmed the practice in TCM of combining remedies with similar functions for their additive and synergistic effects. Following authentication studies, many of the individual TCM herbs and prescriptions were tested for anti-inflammatory and anti-bacterial activity and for their effects on the enzyme CYP3A4. As a result of the bioassays and with consideration of the traditional uses of the herbs, a number have been selected as potential alternatives to the animal products.
7.2. Herbs selected as potential alternatives to animal products
7.2.1. Herbs proposed as potential alternatives to bear bile used in TCM
The following seven species are proposed as potential alternatives to bear bile based on evidence from published TCM and other scientific literature, as well as results from anti-inflammatory and anti-bacterial tests conducted in this study. Of these seven species, five were also highlighted in the IFAW report (1994); Appendix 1 of this report. The five herbs are Zhi Zi, Huang Qin, Huang Bai, Da Huang and Chuan Xin Lian.
- Gardenia jasminoides Ellis (syn.: augusta Merr.) (Rubiaceae) fruit = Zhi Zi
- Scutellaria baicalensis Georgi (Lamiaceae) root = Huang Qin
- Coptis chinensis (Ranunculaceae) rhizome = Huang Lian
- Phellodendron amurense Rupr (Rutaceae) bark = Huang Bai
- Rheum palmatum (Polygonaceae) root and rhizome = Da Huang
- Anemarrhena asphodeloides (Anthericaceae) rhizome = Zhi Mu
- Andrographis paniculata Nees (Acanthaceae) aerial parts = Chuan Xin Lian
7.2.2. Prescriptions proposed as potential alternatives to bear bile used in TCM
Two Kampo medicines are proposed as potential alternatives to bear bile based on published TCM and other scientific literature. Orengedokuto is composed of herbs (1) – (4) listed in Section 7.2.1. Dia-Orengedokuto is composed of herbs (1) – (5) in Section 7.2.1.
7.2.3. Herbs proposed as potential alternatives to rhino horn used in TCM
The following species are proposed as potential alternatives to rhino horn based on evidence from published TCM and other scientific literature, as well as results from anti- inflammatory and / or anti-bacterial tests conducted in this study.
- Scrophularia ningpoensis (Scrophulariaceae) root = Xuan Shen
- Rehmannia glutinosa Steud (Scrophulariaceae) root = Sheng Di Huang
- Paeonia suffruticosa (Paeoniaceae) root = Mu Dan Pi
- Paeonia veitchii Lynch or lactiflora Pall. (Paeoniaceae) root = Chi Shao
- Arnebia euchroma M.Johnst. (Boraginaceae) root = Zi Cao
- Isatis indigotica (Brassicaceae) root = Ban Lan Gen
- Lonicera japonica (Caprifoliaceae) flower bud = Jin Yin Hua
- Forsythia suspensa Vahl (Oleaceae) fruit = Lian Qiao
- Salvia miltiorrhiza Bge (Lamiaceae) root = Dan Shen
7.2.4. Herbs proposed as potential alternatives to tiger bone used in TCM
The following species are proposed as potential alternatives to tiger bone. Herb selection was based on evidence from published TCM and other scientific literature. Further evidence for the potential anti-inflammatory effects of herbs (10) to (12) was obtained from the present study.
- Saposhnikovia divaricata (Turcz.) (Apiaceae) root = Fang Feng
- Clematis chinensis (Ranunculaceae) root and rhizome = Wei Ling Xian
- Angelica pubescens (Apiaceae) root = Du Huo
- Ligusticum chuanxiong (Apiaceae) rhizome = Chuan Xiong
- Gentiana macrophylla (Gentianaceae) root = Qin Jiao
- Epimedium sagittatum (Berberidaceae) aerial parts = Yin Yang Huo
- Atractylodes lancea (Thunb.) or A. chinensis (D.C.) Koidz. (Asteraceae) rhizome = Cang Zhu
- Cinnamomum cassia Don (Lauraceae) bark = Rou Gui
- Morus alba (Moraceae) young branches = Sang Zhi
- Angelica sinensis (Oliv.) Diels (Apiaceae) root = Dang Gui
- Taxillus chinensis (DC.) Danser (Loranthaceae) stem and branch = Sang Ji Sheng
- Atractylodes macrocephala (Asteraceae) rhizome = Bai Zhu
- Spatholobus suberectus (Fabaceae) root and stem = Ji Xue Teng
- Chaenomeles speciosa (Sweet) Nakai (Rosaceae) fruit = Mu Gua
- Cinnamomum cassia (Lauraceae) twigs = Gui Zhi
7.3. Future work
Further research should be undertaken regarding the potential anti-inflammatory activity of the species described above (Section 7.1–7.3). Further studies are therefore warranted to assess other pharmacological mechanisms, using other bioassay systems, through which the plants may mediate their anti-inflammatory effects, in addition to further consultation with TCM practitioners. The results from this study will be disseminated via scientific publications and in the more popular TCM literature. The results from this study should also be discussed with TCM practitioners to determine whether the selected plant species would be considered for use in TCM as substitutes to bear bile, rhino horn and tiger bone.
Source: Research Gate